The product basket of Pradhan Mantri Bhartiya Janaushadhi Pariyojana (PMBJP) comprises of about 1,616 medicines and 250 surgical devices, which are available for sale through more than 8,600 Pradhan Mantri Bhartiya Janaushadhi Kendras (PMBJKs) functional across the country. The product basket covers all major therapeutic groups such as cardiovascular, anti-cancers, anti-diabetics, anti-infectives, anti-allergic, gastro-intestinal medicines, nutraceuticals, etc. A medicine under the Scheme is priced on principle of a maximum of 50% of the average price of the top three branded medicines. Therefore, the price of Jan Aushadhi Medicines is cheaper at least by 50% and in some cases, by 80% to 90% of the market price of branded medicines.
In a month, around 1.25 to 1.50 crore people on an average purchase medicine from more than 8,600 PMBJKs across the country. The annual targets of opening of PMBJKs under the scheme have been achieved within prescribed timelines. The target of having 8,300 PMBJKs by the end of the current financial year, i.e., 2021-22 has already been achieved in the month of September, 2021. As on 28.02.2022, about 8,689 PMBJKs have been opened, covering all districts of the country. State/UT-wise list of PMBJKs is attached as Annexure.
The details of the funds sanctioned, allocated and utilized under the scheme for the financial years 2019-20 to 2021-22 are as under:
(Rs. In cr.)
| Financial Year | Fund Allocated | Fund Utilized |
| 2019-20 | 35.51 | 35.51 |
| 2020-21 | 65.00 | 65.00 |
| 2021-22 (as on 28.02.2022) | 68.50 | 64.65 |
No State/UT-wise specific budget allocation made under the Scheme
The 4th Jan Aushadhi Diwas was celebrated from 1st March, 2022 to 7th March, 2022. During the week-long celebration, various events were organized in coordination with PMBJKs owners, Beneficiaries, States/UTs officials, Public Representatives, Doctors, Health Workers, Nurses, Pharmacists, Jan Aushadhi Mitras and other stakeholders. The day wise activities organized across the country are as under:
| Date | Activity |
| 01.03.2022 | Jan Aushadhi Sankalp Padyatra |
| 02.03.2022 | Matri Shakti Sanman / Swabhiman |
| 03.03.2022 | Jan Aushadhi Bal Mitra |
| 04.03.2022 | Jan Aushadhi Jan Jagran Abhiyan |
| 05.03.2022 | Aao Jan Aushadhi Mitra Bane |
| 06.03.2022 | Jan Aushadhi Jan Arogya Hela (Health Checkup Camps) |
| 07.03.2022 | Jan Aushadi Diwas |
The main event of ‘Jan Aushadhi Diwas’ was held on 7th March, 2022, wherein the Prime Minister interacted through video conferencing with beneficiaries and kendra owners at various locations as well as addressed the citizens.
The Government has set a target to open 10,500 PMBJKs by March 2025, across the country.
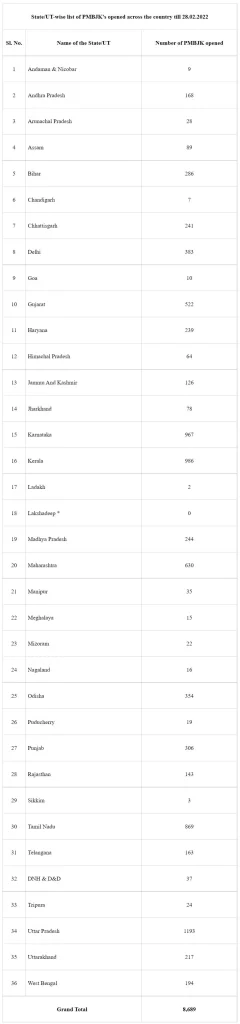
* Medicines are directly supplied to the administration of UT of Lakshadweep
The information was given by the Minister of State for Chemicals and Fertilizers, Shri Bhagwanth Khuba in a written reply in the Lok Sabha today.
Health Ministry’s flagship telemedicine service - “eSanjeevani” records 3 Crore tele-consultationsIndia has crossed a landmark milestone in its eHealth journey. eSanjeevani telemedicine service of Union Health Ministry has crossed 3 crore tele-consultations. Also, “eSanjeevani” telemedicine has set a new record by completing 1.7 lakhs consultations in a day.
In some States, the service is operational on all days of the week and few States are running it round the clock, as well. The telemedicine service contributed considerably during COVID-19 and it decreased load on hospitals and helped patients to digitally/remotely consult medical professionals. This has helped in bridging the rural urban divide by taking quality health services to homes of beneficiaries.
eSanjeevani, first-of-its-kind telemedicine initiative by any country has two variants:
eSanjeevani Ayushman Bharat-Health and Wellness Centre(AB-HWC): A Doctor-to-Doctor telemedicine service under Ayushman Bharat-Health and Wellness Centres scheme of the Government of India, to provide general and specialised health services in rural areas and isolated communities. Doctor-to-Doctor telemedicine service is based on a Hub-and-Spoke model. ‘eSanjeevani AB-HWC’ enables virtual connection between the beneficiary (along with the paramedic and a generalist) at the spoke i.e. HWC and the doctor/specialist at the hub (tertiary healthcare facility/hospital/medical college). This facilitates real-time virtual consultation from doctors & specialists at the hub with the beneficiary (through paramedics) at the spoke. The e-prescription generated at end of the session is used for obtaining medicines. ‘eSanjeevaniAB-HWC’ was implemented with a vision to provide quality health services to maximum number of citizens by leveraging potential of Information Technology bypassing hindrances of geography, accessibility, cost and distance. Currently, eSanjeevaniHWC is operational at around 50,000 Health & Wellness Centres.
eSanjeevaniOPD: This is a patient-to-doctor telemedicine service to enable people to get outpatient services in the confines of their homes. ‘eSanjeevaniOPD’ has also been speedily and widely adopted by citizens in all parts of the country. It is available as a mobile app for both Android and iOS based smart phones, and these apps have seen over 3 million downloads.
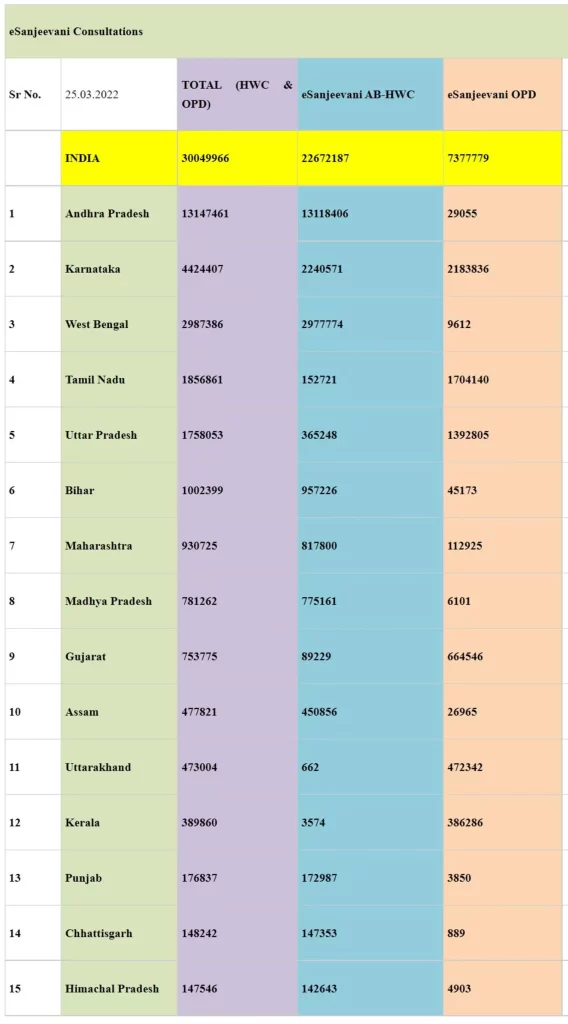
Of the 3 crore beneficiaries, 2,26,72,187 have been served through eSanjeevaniAB-HWC portal while 73,77,779 have availed the benefits through eSanjeevaniOPD. Over 1,00,000 doctors, specialists etc., have been onboarded to serve beneficiaries on the National Telemedicine Service. The substantial number of consultations through ‘eSanjeevaniAB-HWC’ indicates that rural India has embraced the use of digital health technologies. It further strengthens the aim of Ayushman Bharat scheme which strives for Universal Health Coverage by providing universal, free and quality healthcare closer to people’s homes.
eSanjeevaniOPD now enables creation of Ayushman Bharat Health Account (ABHA), which will facilitate access and shareability of health data with consent of the beneficiary, with participating healthcare providers and beneficiaries as per Ayushman Bharat Digital Mission (ABDM).
eSanjeevani is an exemplification of the ‘Make in India’ initiative as it has been developed indigenously by the Health Informatics Group in Mohali branch Centre for Development and Advanced Computing (C-DAC) a number of experienced engineers are providing constant backend technical and operational support to ensure high throughput and high uptime; the National Telemedicine Service is operational with over 99.5% uptime. eSanjeevani is now being augmented further by the Health Informatics Group in the Mohali’s branch of Centre for Development of Advanced Computing. AI-led interventions are being conceptualized to enhance the convenience and efficacy of the service. Services to support more than 10 lakhs consultations per day in the very near future are in the offing.
Witnessing the success of National Telemedicine Service of MHFW and quick adoption of telemedicine in the country, Ministry of Defence has rolled out SeHATOPD - Services eHealth Teleconsultation & Assistance - a telemedicine portal for defense personnel. SeHATOPD specifically serves defence personnel and their dependents. Soon, SeHATOPD will be integrated with Ex-Servicemen Contributory Health Scheme (ECHS) to make the benefits of tele-consultation easily accessible to the veterans and their families. National AIDS Control Organisation (NACO) and Alliance India are working on a dedicated national telemedicine platform (eHIVCare) for people living with HIV/AIDS. It will also operate along the same lines as eSanjeevani in terms of technology but will be customised in a way that caters to the particular needs of HIV/AIDS patients in order to augment a better and more comfortable quality of treatment to them.
10 States that are leading in terms of adoption of eSanjeevani are Andhra Pradesh (13147461), Karnataka (4424407), West Bengal (2987386), Tamil Nadu (1856861), Uttar Pradesh (1758053), Bihar (1002399), Maharashtra (930725), Madhya Pradesh (781262), Gujarat (753775) and Assam (477821).
Union Health Minister, Dr Mansukh Mandaviya will inaugurate the Step - Up to End TB- World TB Day Summit on the occasion of World TB Day (24th March 2022) at Vigyan Bhawan, New Delhi. Chief Guest at the Summit will be the Hon’ble Governor of Uttar Pradesh, Smt. Anandiben Patel, who will attend virtually. Leading discussions from the front, she will bring to light India’s accelerated pace of innovations and achievements for eliminating TB by 2025. The Union Minister of State for Health and Family Welfare, Dr Bharati Pravin Pawar will also be present at the summit.
In March 2018, Hon’ble Prime Minister Shri Narendra Modi chaired the Delhi End TB Summit. At the Summit, the Prime Minister gave the clarion call to End TB in India by 2025, five years ahead of the TB-related SDG targets of 2030.
The Ste-Up to End World TB Day Summit of 24th March 2022 is not only a follow-up to 2018 that gauges how far – and to what degree – India has progressed in its journey to TB elimination; it is also a reiteration of India’s TB commitments, and an effort to assemble the right minds as the country moves forward to meet its TB elimination objectives. The Summit will provide a forum to showcase the National TB Elimination Programme’s learnings and successes and frame it in a manner that inspires more forward-looking policies across infectious diseases, and not just TB alone. From vaccine development to the need for greater inter-departmental/ministerial and inter-state collaborations, the event aims to be an incubator for TB mitigation ideas that are disruptive and cognizant of a changing post-COVID world order.
At the event, Union Health Minister will award well-performing states and districts for achieving improved levels of TB elimination. A TB survivor will share her story and journey of overcoming this disease.
Featuring a meeting with State Health Ministers, the Hon’ble Health Minister will lead a session eliciting experience-sharing and commitments to intensify elimination efforts at the state and district level, with parallel sessions for states to present their best practices. The Summit will then lead into a session on findings from the to-be-released National TB Prevalence Survey results, with an eye for India’s action plan for achieving SDG elimination targets. To give an experiential look into the TB landscape, development partner organizations will present select exhibitions on innovative program practices, and give attendees a keen look into India’s future of becoming TB-free through a whole-of-society approach.
The event will further call for a Jan Andolan by eliciting commitments across Ministries and states, as well as setting the agenda for elected representatives and grassroots leaders to provide leadership at the last mile.
To be held over two days, this Summit will be attended by Health Ministers from various states, State Health officials and other key stakeholders working on the issue of TB elimination in India.
As informed by Department of Revenue, Specified Drugs, Medicines and vaccines attract 5% GST and Other medicines, in general attract 12% GST. Serial No.173 to 181 of notification No. 1/2017-Central Tax (Rate) provides 5% GST on specified drugs and medicines. The associated list of drugs and medicines is available at (https://egazette.nic.in/WriteReadData/2017/176965.pdf Page No.239-306).
Further, as informed by Department of Pharmaceuticals, pursuant to notification of the National Pharmaceutical Pricing Policy (NPPP) on 7th December, 2012, the Government has notified the Drugs (Prices Control) Order, 2013 (DPCO-2013) with an objective to put in place a regulatory framework for pricing of drugs so as to ensure the availability of essential medicines at reasonable prices.
As per provisions of DPCO, 2013, the ceiling price of all scheduled formulations figuring in the National List of Essential Medicines (NLEM) issued by the Ministry of Health & Family Welfare are fixed by the National Pharmaceutical Pricing Authority (NPPA) under the Department of Pharmaceuticals. All manufacturers of these scheduled drugs are required to sell their products at a price equal to or lower than the ceiling price. Further, NPPA monitors the prices of non-scheduled drugs so as to ensure that increase in their Maximum Retail Price (MRP) is not more than 10% of what was prevalent during the preceding twelve months. The details of various medicines and medical devices under price control is available at the website of NPPA, i.e., www.nppaindia.nic.in.
The Union Minister of State for Health and Family Welfare, Dr. Bharti Pravin Pawar stated this in a written reply in the Rajya Sabha today.
The National Health Policy formulated in 2017 envisages to provide universal access to good quality health care services through increasing access, increasing affordability by lowering the cost of healthcare delivery and equity. The policy envisages as its goal the attainment of the highest possible level of health and well-being for all at all ages, through a preventive and promotive health care orientation in all developmental policies, and universal access to good quality health care services without anyone having to face financial hardship as a consequence. The Policy is centered on the key principles of Equity; Affordability; Universality; Patient Centeredness & Quality of care; accountability, Inclusive partnerships; Pluralism and decentralization.
Public Health and Hospitals is under the State List. The Central Govt. has taken several initiatives for supplementing the efforts of the State for providing quality and affordable healthcare services to the people.
Under National Health Mission, the Government has taken many steps towards universal health coverage, by supporting the State Government in providing accessible & affordable healthcare to people. It encompasses the National Rural Health Mission (NRHM) and the National Urban Health Mission (NUHM) as its two Sub-Missions. Under the National Health Mission, financial and technical support is provided to States/UTs to provide accessible, affordable and quality healthcare, especially to the poor and vulnerable sections of the population, in both urban and rural areas. The National Health Mission provides support for improvement in health infrastructure, availability of adequate human resources to man health facilities, to improve availability and accessibility to quality health care especially for the underserved and marginalized groups in rural areas.
Government has launched four mission mode projects, namely PM-Ayushman Bharat Health Infrastructure Mission (PM-ABHIM), Ayushman Bharat Health & Wellness Centres (ABHWCs), Pradhan Mantri Jan ArogyaYojana (PMJAY) and National Digital Health Mission (NDHM).
PM-ABHIM was launched as a mission to develop the capacities of primary, secondary, and tertiary care health systems, strengthen existing national institutions, and create new institutions, to cater to detection and cure of new and emerging diseases. The PM-ABHIM is a Centrally Sponsored Scheme with some Central Sector Components, for implementation of the Atmanirbhar Bharat Package for health sector with an outlay of Rs 64,180 crore.
Under Ayushman Bharat Health & Wellness Centres (HWCs), Comprehensive Primary healthcare by strengthening Sub Health Centres (SHCs) and Primary Health Centres (PHCs) are to be facilitated. The HWCs are to provide preventive, promotive, rehabilitative and curative care for an expanded range of services encompassing Reproductive and child care services, Communicable diseases, Non-communicable diseases, Palliative care and elderly care, Care for common mental disorders, neurological conditions (epilepsy, dementia) and substance use disorders management (tobacco, alcohol, drugs), Oral health, ENT care, and Basic emergency care.
To every citizen to get health card; a Ayushman Bharat Digital Mission (ABDM) has been announced on 27th September, 2021 with aim to develop the backbone necessary to support the integrated digital health infrastructure of the country. The objective of the mission is to bridge the existing gap amongst different stakeholders of Healthcare ecosystem through digital highways.
The Union Minister of State for Health and Family Welfare, Dr. Bharti Pravin Pawar stated this in a written reply in the Rajya Sabha today.
As per the National Mental Health Survey conducted by the National Institute of Mental Health and Neurosciences (NIMHANS), Bangalore in 12 States of the country, the prevalence of mental disorders including common mental disorders, severe mental disorders, and alcohol and substance use disorders (excluding tobacco use disorder) in adults over the age of 18 years is about 10.6%. The major findings of the survey are as under:
The prevalence of mental morbidity is high in urban metropolitan areas.
Mental disorders are closely linked to both causation and consequences of several non-communicable disorders (NCD).
Nearly 1 in 40 and 1 in 20 persons suffer from past and current depression, respectively.
Neurosis and stress related disorders affect 3.5% of the population and was reported to be higher among females (nearly twice as much in males).
Data indicate that 0.9 % of the survey population were at high risk of suicide.
Nearly 50% of persons with major depressive disorders reported difficulties in carrying out their daily activities.
Realizing the impact that COVID-19 may have on the mental health of the people, the Government has taken a number of initiatives, including -
Setting up of a 24/7 helpline to provide psychosocial support, by mental health professionals, to the entire affected population, divided into different target groups viz children, adult, elderly, women and healthcare workers. Till date a total of 5,77,743 calls have been received on the helpline.
Issuance of guidelines/ advisories on management of mental health issues, catering to different segments of the society.
Advocacy through various media platforms in the form of creative and audio-visual materials on managing stress and anxiety, and promoting an environment of support and care for all.
Issuance and dissemination of detailed guidelines by the National Institute of Mental Health and Neurosciences (NIMHANS), Bengaluru- "Mental Health in the times of COVID-19 Pandemic - Guidance for General Medical and Specialized Mental Health Care Settings".
All the guidelines, advisories and advocacy material can be accessed on Ministry of Health and Family Welfare website under “Behavioural Health – Psychosocial helpline” (https://www.mohfw.gov.in/).
Online capacity building of health workers by NIMHANS in providing psychosocial support and training through (iGOT)-Diksha platform.
Further, with a view to provide affordable and accessible mental healthcare facilities, the Government is implementing the National Mental Health Programme (NMHP) in the country. The District Mental Health Programme (DMHP) component of the NMHP has been sanctioned for implementation in 704 districts for which support is provided to States/UTs through the National Health Mission. Facilities made available under DMHP at the Community Health Centre (CHC) and Primary Health Centre (PHC) levels, include outpatient services, assessment, counselling/ psycho-social interventions, continuing care and support to persons with severe mental disorders, drugs, outreach services, ambulance services etc. In addition to above services there is a provision of 10 bedded in-patient facility at the District level.
Besides the above, the Government has announced a “National Tele Mental Health Programme” in the Budget of 2022-23, to further improve access to quality mental health counselling and care services in the country.
To generate awareness among masses about mental illnesses Information, Education and Communication (IEC) activities are an integral part of the NMHP. At the District level, sufficient funds are provided to each District under the DMHP under the Non-communicable Diseases flexi-pool of National Health Mission for IEC and awareness generation activities in the community, schools, workplaces, with community involvement. Under the DMHP various IEC activities such as awareness messages in local newspapers and radio, street plays, wall paintings etc. are undertaken by the States/UTs.
The Union Minister of State for Health and Family Welfare, Dr. Bharti Pravin Pawar stated this in a written reply in the Rajya Sabha today.
The Covaxin and Covishield are two different types of Covid-19 vaccine and their manufacturing processes are also different. The price of vaccine for procurement by Government of India is negotiated by National Expert Group on Vaccine Administration for COVID-19 (NEGVAC) and its subgroups involving detailed deliberations with the vaccine manufacturers. Under National COVID-19 Vaccination Programme, COVID-19 vaccine is available free of cost at Government COVID-19 Vaccination Centres (CVCs) to all eligible beneficiaries irrespective of their socio-economic status.
The vaccine manufacturers are free to fix the price of vaccine for procurement by Private Hospitals which has to be declared in a transparent manner. However, Government of India has fixed a maximum service charge of INR 150 per dose over and above the price of vaccine for vaccine administration at Private COVID-19 Vaccination Centres (CVCs). State Governments have been advised to monitor the price charged at the private hospitals.
The Union Minister of State for Health and Family Welfare, Dr. Bharti Pravin Pawar stated this in a written reply in the Rajya Sabha today.
As per the WHO Global Data on Visual Impairment 2010, India (20.5%) along with China (20.9%) were among the most affected countries by blindness in the world; however, since then our country has made significant improvement. The WHO Global Action Plan for Universal Eye Health 2014-2019 targets a reduction in the prevalence of Avoidable Visual Impairment (defined as presenting visual acuity less than 6/18 in better eye) by 25% by the year 2019 from the baseline level of 2010. The WHO had estimated a prevalence of blindness and Visual Impairment (VI) as 0.68% and 5.30% respectively in India for the year 2010. The recent survey shows a reduction in blindness by 47.1% (from 0.68% to 0.36%) and 51.9% in VI (from 5.30%to 2.55%). Thus, target of 25% reduction in visual impairment has been successfully achieved by India.
The key reasons for high burden of cataract blindness in India are:
Increasing elderly population due to improved life expectancy in country and cataract is age related disease.
High prevalence is observed due to more exposure to Ultra Violet radiations (as indicated by ICMR- UVR study)
The targets were affected in last two years due to Covid 19 pandemic in the country
Lack of awareness in remote areas about the availability of treatment among population.
Limited access to treatment facilities in remote areas.
A wide variance in cataract surgery rates from state to state revealing the need to set up cataract treatment facilities specific areas.
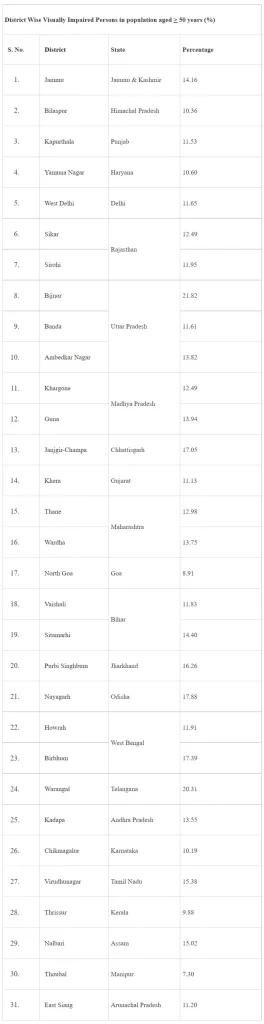
The National Blindness &Visual Survey India 2015-19 was conducted using Rapid Assessment of Avoidable Blindness (RAAB) strategy in 31 districts randomly selected from 24 states/UT’s by Dr. RP Centre AIIMS to provide evidence about present status of blindness and visual impairment in the country. It included both urban and rural districts. The percentage of Visually Impaired Persons in population > 50 years in 31 districts randomly selected from 24 states /UT’s is at Annexure-I.
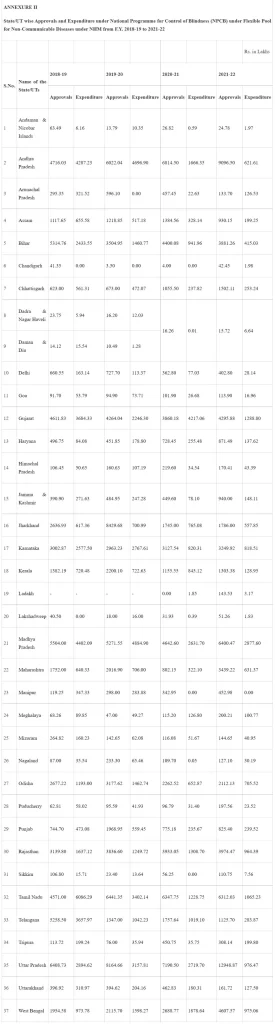
The National Programme for Control of Blindness & Visual Impairment (NPCB&VI) was launched in 1976to provide comprehensive eye care to all citizens across all districts of the country. Under NPCB&VI funds allocated during last three years and the current year, State/UT wise is placed at Annexure-II.
Eye donation is one of the approved activities under the National Programme for Control of Blindness and Visual Impairment (NPCB&VI). Non-recurring grant-in-aid (GIA) is provided to Eye Banks in public sectors up to Rs. 40.00 Lakh per unit and to Eye Donation Centers in public sector up to Rs. 1.00 Lakh per unit for strengthening/ development.
Recurring GIA to Eye Banks is paid under NPCB&VI at the rate of Rs. 2000/- per pair of eyes (Eye Banks reimburse the Eye Donation Centers attached with it for eye collected by them @ Rs. 1000/- per pair of eyes) to meet the cost of consumables including preservative material & media, transportation and contingencies- I
IEC activities are held which include observing Eye Donation Fortnight as well. Financial support is provided to States/ UTs for undertaking IEC activities.
This Ministry has funded a project by Dr. R. P. Centre for Ophthalmic Sciences, AIIMS, New Delhi – "Development and Supply of Longer Storage Corneal Preservation Media Along with the Regular Supply of Corneal Storage Media to Indian Eye Bank”, which essentially provides support for supply of M. K. Medium – a preservative medium for donated cornea.
Annexure-I
The Union Minister of State for Health and Family Welfare, Dr. Bharti Pravin Pawar stated this in a written reply in the Rajya Sabha today.
“Given India has one of the world’s largest vaccine manufacturing industries which supplies vaccines to more than 150 countries and meets 65-70% of WHO’s vaccine requirements, India is willing to offer its robust vaccine manufacturing industry for developing vaccines for BRICS (Brazil, Russia, India, China and South Africa) countries as well as the world.” Union Minister of Health and Family Welfare, Dr. Mansukh Mandaviya said as he launched the BRICS Vaccine R&D Center and Workshop on Vaccine Cooperationthrough video-conference, here today.
Dr. Mandaviya highlighted that “This Centre will help to pool together complementary advantages of BRICS countries in vaccine research and development and boost the capacity of BRICS countries to prevent and control infectious diseases and provide timely help to other developing countries in need.” It will should entail basic R&D, preclinical &clinical studies and strengthen BRICS countries laboratory capacities to develop and standardize assays for testing vaccine candidates. He added that “The Centre will be instrumental in streamlining vaccination resources and facilitate equitable access to safe and efficacious COVID-19 vaccines”.
The Union Health Minister highlighted that the “BRICS Vaccine R&D Centre is a welcome initiative to collaborate with countries, share experiences, build collaborations for mutual benefits and accelerate development of vaccine of public health importance. This will enable saving lives and livelihood to propel us towards economic recovery for the citizens of BRICS countries and the world.”
At the virtual launch, Dr. Mansukh Mandaviya conveyed his gratitude and appreciation towards BRICS countries for collectively undertaking scientific efforts towards research and development of vaccines. “Amidst a global pandemic, I appreciate BRICS presidency for coordinating the launch of this Centre. This is a testament of the commitment of BRICS countries towards global pandemic response”, he stated. The Union health Minister applauded all those who have worked towards vaccine research and development. “I would like to convey my gratitude and appreciation for the relentless efforts of health professionals, scientists, researchers, drug regulatory authorities, and policy makers locally and globally, who have served as the backbone of the health system and vaccine development since the onset of pandemic”. He further stated that development and approval of safe and effective vaccines for COVID-19 in less than a year after the emergence of theCOVID-19 virus is an incredible scientific achievement and has shown us about what is possible in future vaccine development.”
Dr. Mandaviya stated that WHO’s R&D blueprint and International Health Regulations should be the guiding principles for this Centre and further proposed that “BRICS countries should work together to support endeavors such as ACT-A, COVAX, CEPI, etc., to achieve the WHO’s laid target of vaccinating 70% of the world’s population with COVID-19 vaccines by mid-2022.” He added that “apart from pandemic and health emergencies, there is an ample scope of collaboration among countries like in the field of vaccine preventable diseases with high morbidity and mortalityand for those diseases withno vaccines available currently such as AIDS, TB etc.”
Elaborating on the country’s capabilities and success of the world’s largest COVID-19 vaccination drive, Dr. Mandaviya said that India has so far administered of more than 1.81 billion vaccination doses. This wouldn’t have been possible without a robust and favorable ecosystem of vaccine R&D in the country, he stressed. “India has also so far approved 9 vaccines for COVID-19 emergency use, of which 5 are indigenous. This also involves world’s first of a kind m-RNA vaccine Gennova that has been developed indigenously, and produced outside WHO transfer technology program”. He said that vaccine industry in India functions in a dual mode—De-novo product development i.e., within the country and technology transfer through local-global partnership. He invited stakeholders to collaborate with India as “we have prioritised strengthening vaccine research and development efforts for diseases of local as well as global relevance.”
With the commitment of BRICS countries towards strengthening their cooperation in various fields, special emphasis was given to vaccine research and development. In this regard, a BRICS Vaccine R&D Centre was proposed to be established in 2018 Johannesburg Declaration. Over the years and especially throughout the pandemic, this process was expedited and finally in New Delhi Declaration of XIII BRICS Summit, leaders reiterated their commitment towards the early launch of BRICS Vaccine R&D Centre in virtual format.
With the support from the BRICS governments, each BRICS country has also identified their national centers, namely Immunobiological Technology Institute (Biomanguinhos) of the Oswaldo Cruz Foundation (Fiocruz), Smorodintsev Research Institute of Influeza, Indian Council of Medical Research (ICMR), Sinovac Life Sciences Co. Ltd, South African Medical Research Council.
The ceremony was chaired by Mr. Wang Zhigang, Minister of Science and Technology, People’s Republic of China who urged countries to focus upon promoting fair and equitable distribution of vaccines and to promote synergies among BRICS countries through this centre and other such initiatives. Apart from cooperation in vaccine R&D and their experiences in COVID-19 management, the panel discussed strategies to deal with future pandemics cooperatively among BRICS countries.
The meeting was attended by Mr. Marcelo Queiroga (Health Minister, Brazil), Mr. Mikhail Murashko (Health Minister, Russia), Dr Blade Nzimande (Minister of Higher Education, Science and Innovation, South Africa), delegates, senior representatives and research experts from BRICS countries.
Union Health Secretary, Shri Rajesh Bhushan chaired a meeting through video conference (VC) today with all States and UTs to review the operationalisation status of Ayushman Bharat Health & Wellness Centres (HWCs), Tele-consultation services and physical and financial progress made under ECRP-II and Prime Minister Atmanirbhar Swasth Bharat Yojana (PM-ABHIM).

Highlighting that Government of India is dedicated to expanding public healthcare delivery across the country, States were informed through a detailed presentation on the status of implementation of AB-HWCs, their operationalisation as tele-consultation centres, and status of implementation of projects under ECRP-II package.
Union Health Secretary highlighted that for ensuring comprehensive Primary Health Care (CPHC) under Ayushman Bharat, Sub Health Centres (SHCs) and Primary Health Centres (PHCs) are being strengthened as Health and Wellness Centres (HWCs). The HWCs are crucial in providing preventive, promotive, rehabilitative and curative care for an expanded range of services encompassing reproductive and child health services, communicable diseases, non-communicable diseases, palliative care and elderly care, oral health, ENT care, and basic emergency care. Trained officials like Mid-level Health Care Provider (MLHP)/Community Health Officer (CHO) are being placed at HWC-SHC and Medical Officer at PHC (Rural/Urban). They would facilitate delivery of these services at their respective health centres. HWCs will be crucial in enhancing continuum of care and tele-health/ referrals.
The States were advised to ensure operationalisation of target of 1.10 lakh HWCs by 31st March 2022 through customised and focused strategy. This in effect means that these HWCs must be fully functional and equipped to dispense free meds, provide free diagnostics and all prescribed health packages including yoga and healthy living sessions.
They were also advised to ensure that all the 1.10 lakh AB-HWCs are adequately equipped to function as effective and vibrant tele-consultation “Spokes”. This would include ensured availability of internet connectivity, desktop/ laptop and required trained and skilled personnel including CHO. States also are required to ensure that all the HWCs are mapped to a “Hub” which could be a District Hospital or District Medical College Hospital. For each such spoke, States must ensure that a base minimum number teleconsultation sessions are conducted, starting from today.
Reiterating the advise to states on expediting utilisation of funds released under ECRP-II package for strengthening healthcare infrastructure across the country (since the funds will lapse on 31st March 2022), States were again reminded to accelerate completion of projects under ECRP-II, such that subsequent instalment of funds can be released by Union Health Ministry. They were also informed that necessary exemption from ECI have been taken and formally communication to the poll-bound States for utilisation of funds.
Additionally, States were also advised that they can utilise savings under certain components of ECRP-II package with due approval of State Health Societies for permissible and admissible components, instead of again seeking approval of Union Health Ministry.
States were also requested to expedite proposals and MOUs to be sent to Union Health Ministry under PM-ABHIM to enable the Ministry to release funds for the states. States were advised to review the progress under this too.
Shri Vikas Sheel, AS & MD, Shri Vishal Chauhan, Jt. Secy, Shri Lav Agarwal, Jt. Secy and other senior officers of Union Health Ministry were present in the virtual review meeting along with NHM Mission Directors and other officials from States/UTs.
