Government has notified the Drugs and Cosmetics (Second Amendment) Rules, 2020 to support the National Blood Policy. These Rules pertain to functioning of Blood Banks, Blood processing and related matters. The copy of the Rules is available at web link: https://cdsco.gov.in/opencms/opencms/system/modules/CDSCO.WEB/elements/download_file_division.jsp?num_id=NTc2MQ
The Government is also taking up the matter regarding processing charges of blood and blood components with the National Pharmaceutical Pricing Authority (NPPA) for bringing the same under Drugs Prices Control Order (DPCO).
During a meeting with the State Blood Transfusion Councils (SBTCs) of all States and Union Territories (UTs) held on 03rd January, 2022, it has been recommended to take up a review of the National Blood Policy. Further, the NBTC/BTS Division is under transition from National AIDS Control Organization (NACO) to Directorate General of Health Services (Dte.GHS).
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the RajyaSabha today.
According to the study report “India: Health of the Nation's States”- The India State-Level Disease Burden Initiative in 2017 by Indian Council of Medical Research (ICMR), it is estimated that the proportion of deaths due to Non-Communicable Diseases (NCDs) in India have increased from 37.9% in 1990 to 61.8% in 2016. The four major NCDs are cardiovascular diseases (CVDs), cancers, chronic respiratory diseases (CRDs) and diabetes which share four behavioral risk factors –unhealthy diet, lack of physical activity, and use of tobacco and alcohol.
The detailed proportion changes in Disability Adjusted Life Years (DALYs) number for the leading individual causes of these NCDs among women from 1990 to 2016 are given in the table below:
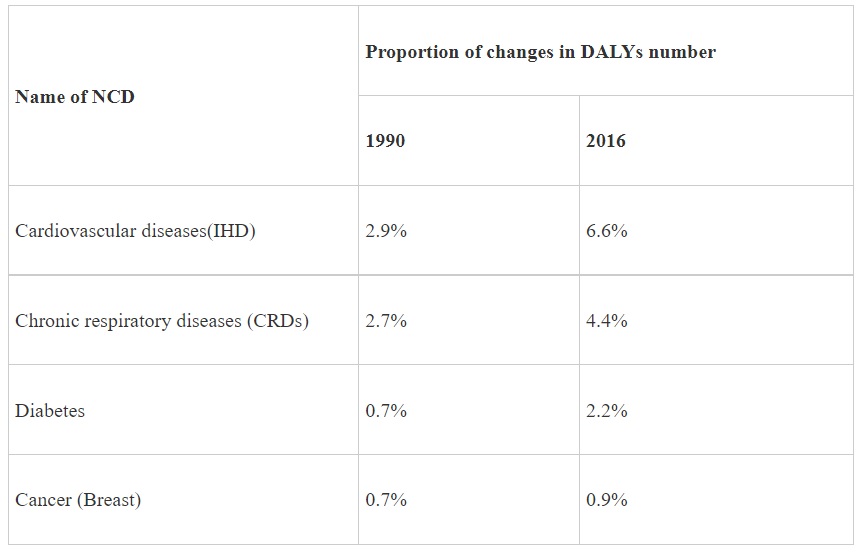
Health is a state subject. The Department of Health & Family Welfare, Government of India, however, provides technical and financial support to the States/UTs under the National Programme for Prevention and Control of Cancer, Diabetes, Cardiovascular Diseases and Stroke (NPCDCS), (launched in 2010) as part of National Health Mission (NHM), based on the proposals received from the States/UTs and subject to the resource envelope. The programme focuses on strengthening infrastructure, human resource development, health promotion & awareness generation for prevention, early diagnosis, management and referral to an appropriate level of healthcare facility for treatment of the Non-Communicable Diseases (NCDs).
Under NPCDCS, 677 NCD clinics at District level, 187 District Cardiac Care Units, 266 District Day Care Centres and 5392 NCD clinics at Community Health Centre level have been set up to ensure the treatment of common NCDs.
A population-based initiative for prevention, control and screening for common Non-Communicable Diseases (NCDs) i.e. diabetes, hypertension and common cancers has been rolled out in the country under NHM and also as a part of Comprehensive Primary Health Care. Under the initiative, persons more than 30 years of age are targeted for their screening for the common NCDs, in which there is focus on screening of breast cancer and cervical cancer among women. Screening of these common NCDs is an integral part of service delivery under Ayushman Bharat – Health and Wellness Centres.
Preventive aspect of NCDs is strengthened under Comprehensive Primary Health Care through Ayushman Bharat Health Wellness Centre scheme, by promotion of wellness activities and targeted communication at the community level. Other initiatives for increasing public awareness about NCDs and for promotion of healthy lifestyle includes observation of National & International Health Days and use of print, electronic and social media for continued community awareness. Furthermore, healthy eating is also promoted through FSSAI. Fit India movement is implemented by Ministry of Youth Affairs and Sports, and various Yoga related activities are carried out by Ministry of AYUSH. In addition, NPCDCS gives financial support under NHM for awareness generation (IEC) activities for NCDs to be undertaken by the States/UTs as per their Programme Implementation Plans (PIPs).
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Rajya Sabha today.
According to the study report “India: Health of the Nation's States”- The India State-Level Disease Burden Initiative in 2017 by Indian Council of Medical Research (ICMR), it is estimated that the proportion of deaths due to Non-Communicable Diseases (NCDs) in India have increased from 37.9% in 1990 to 61.8% in 2016. The four major NCDs are cardiovascular diseases (CVDs), cancers, chronic respiratory diseases (CRDs) and diabetes which share four behavioral risk factors –unhealthy diet, lack of physical activity, and use of tobacco and alcohol.
The detailed proportion changes in Disability Adjusted Life Years (DALYs) number for the leading individual causes of these NCDs among women from 1990 to 2016 are given in the table below:
Health is a state subject. The Department of Health & Family Welfare, Government of India, however, provides technical and financial support to the States/UTs under the National Programme for Prevention and Control of Cancer, Diabetes, Cardiovascular Diseases and Stroke (NPCDCS), (launched in 2010) as part of National Health Mission (NHM), based on the proposals received from the States/UTs and subject to the resource envelope. The programme focuses on strengthening infrastructure, human resource development, health promotion & awareness generation for prevention, early diagnosis, management and referral to an appropriate level of healthcare facility for treatment of the Non-Communicable Diseases (NCDs).
Under NPCDCS, 677 NCD clinics at District level, 187 District Cardiac Care Units, 266 District Day Care Centres and 5392 NCD clinics at Community Health Centre level have been set up to ensure the treatment of common NCDs.
A population-based initiative for prevention, control and screening for common Non-Communicable Diseases (NCDs) i.e. diabetes, hypertension and common cancers has been rolled out in the country under NHM and also as a part of Comprehensive Primary Health Care. Under the initiative, persons more than 30 years of age are targeted for their screening for the common NCDs, in which there is focus on screening of breast cancer and cervical cancer among women. Screening of these common NCDs is an integral part of service delivery under Ayushman Bharat – Health and Wellness Centres.
Preventive aspect of NCDs is strengthened under Comprehensive Primary Health Care through Ayushman Bharat Health Wellness Centre scheme, by promotion of wellness activities and targeted communication at the community level. Other initiatives for increasing public awareness about NCDs and for promotion of healthy lifestyle includes observation of National & International Health Days and use of print, electronic and social media for continued community awareness. Furthermore, healthy eating is also promoted through FSSAI. Fit India movement is implemented by Ministry of Youth Affairs and Sports, and various Yoga related activities are carried out by Ministry of AYUSH. In addition, NPCDCS gives financial support under NHM for awareness generation (IEC) activities for NCDs to be undertaken by the States/UTs as per their Programme Implementation Plans (PIPs).
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Rajya Sabha today.
India has completed its transition from iodine deficiency to iodine replete status. It is believed that iodine supplementation can cause a spurt in autoimmune thyroid dysfunction and hypothyroidism, by making the thyroid gland more susceptible to damage by body’s own immune system. The prevalence of self-reported goitre or thyroid disorder in National Family Health Survey IV [NFHS IV (2015-2016)] was 2.2%, while it was 2.9% in NFHS-V (2019-2021).
The NFHS IV (2015-2016) has reported that amongst individuals between the age 15-49 years, the self-reported prevalence of goitre or thyroid disorder was nearly 2% in females and less than 1% in males. Also, the reported prevalence increased with age in women (15-19 years: 0.7%; 20-34 years: 1.8%; 35-49 years: 3.4%). As per NFHS V, the details of States/UTs wise cases reported are given below.

As per the NFHS IV (2015-2016), amongst 6,99,686 women in their reproductive age groups (15-49 years), those in the highest quintile of wealth index had three to four-fold higher risk of having thyroid disorders. In addition, there was a graded increase in risk of having thyroid disorders from poorest to richest.
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the RajyaSabha today.
“India is implementing the largest immunisation programme globally where we annually cover more than 3 crore pregnant women and 2.6 crore children through the Universal Immunisation Programme (UIP)”. Dr. Mansukh Mandaviya, Union Minister of Health and Family Welfare stated while launching Intensified Mission Indradhanush (IMI) 4.0 virtually today in presence of health officials of States and Union Territories. Shri Keshab Mahanta, Health Minister of Assam and Shri Rushikesh Patel, Health Minister of Gujarat virtually participated.
Intensified Mission Indradhanush 4.0 will have three rounds and will be conducted in 416 districts (including 75 districts identified for Azadi ka Amrit Mahotsav) across 33 States/UTs in the country. In the first round (Feb-April 2022), 11 states will conduct IMI 4.0. These are Assam, Uttarakhand, Gujarat, Jammu & Kashmir, Meghalaya, Mizoram, Nagaland, Rajasthan, Sikkim, Tripura and Chhattisgarh. The others (22 states) will conduct the rounds from April to May 2022. These states/UTs include Himachal Pradesh, Maharashtra, Andhra Pradesh, Manipur, Arunachal Pradesh, Odisha, Bihar, Puducherry, Delhi, Punjab, Goa, Tamil Nadu, Haryana, Telangana, Jharkhand, Dadra & Nagar Haveli and Daman & Diu, Karnataka, Uttar Pradesh, Kerala, West Bengal, Madhya Pradesh, A & N Islands.
On the occasion, the Union Health Minister saluted the commitment and dedication of the frontline vaccinators who brave difficult terrain and weather to ensure that the farthest village and household are covered with the protection of vaccines. “The health care workers are providing a great service to the nation. Their dedication is an inspiration to me and to others for contributing to nation building”, he added.

Dr. Mandaviya expressed satisfaction that our efforts have been reflected in the latest National Family Health Survey which has indicated increased coverage. “Vaccines are one of the most effective, affordable and safe methods to protect infants, children and pregnant women from diseases and mortality. With the aim to increase the Full Immunisation Coverage, Hon. Prime Minister launched Mission Indradhanush in December 2014 to cover the partially and unvaccinated pregnant women and children in pockets of low immunization coverage, high-risk and hard-to-reach areas and protect them from vaccine preventable diseases”, he said. Under Mission Indradhanush, all vaccines under Universal Immunization Program (UIP) are provided as per National Immunization Schedule. Mission Indradhansuh was also identified as one of the flagship schemes under Gram Swaraj Abhiyan (16,850 villages across 541 districts) and Extended Gram Swaraj Abhiyan (48,929 villages across 112 aspirational districts).
Dr. Mandaviya noted that while pace of routine immunization has slowed down due to COVID pandemic, IMI 4.0 will immensely contribute in filling the gaps and make lasting gains towards Universal Immunization. It will ensure that Routine Immunization (RI) services reach the unvaccinated and partially vaccinated children and pregnant women, he added.
Highlighting the important role of vaccines in public health, the Union Health Minister highlighted the achievements of the country-wide COVID19 vaccination drive under which around 170 crore doses of COVID vaccines have been administered till date. This achievement of India has been acknowledged and applauded globally, he added. He emphasised on the need of “Sabka Prayas” and “Jan Lok Bhaagidaari” to achieve the goal of universal immunisation in the country. “Only with the collective and collaborative efforts of the Centre, the States and beneficiaries shall we be able to achieve the target of full immunization coverage in the country”, he stated. He urged the States to work holistically at different levels, coordinating with district administration, panchayats and the urban local bodies.
The Union Health Minister virtually launched the IMI 4.0 portal and released the “Operational Guidelines for IMI 4.0”, “Strengthening Immunization in Urban Areas-A framework for Action” and a handbook for “Mahila Arogya Samiti on Urban Immunization” and awareness material/IEC package developed as part of the campaign.
Till date, ten phases of Mission Indradhanush have been completed covering 701 districts across the country. As of April 2021, during the various phases of Mission Indradhanush, a total of 3.86 crore children and 96.8 lakh pregnant women have been vaccinated. The first two phases of Mission Indradhanush resulted in 6.7% increase in full immunization coverage in a year. A survey (IMI- CES) carried out in 190 districts covered in Intensified Mission Indradhanush (5th phase of Mission Indradhanush) shows 18.5% points increase in full immunization coverage as compared to NFHS-4. As a result of continuous efforts over the years for strengthening routine immunization and immunization intensification drives conducted from time to time, the immunization coverage has shown a considerable improvement as per the latest reports of National Family Health Survey (2019-21) as compared to National Family Health Survey -4(2015-16). The Full Immunization Coverage among children aged 12-23 months of age has increased from 62% (NFHS-4) to 76.4% (NFHS-5).
Three rounds of IMI 4.0 have been planned to catch up on the gaps that might have emerged due to the COVID-19 pandemic. The activity will be conducted in 416 districts across 33 states/UTs. These districts have been identified based on vaccination coverage as per the latest National Family Health Survey-5 report, Health Management Information System (HMIS) data and burden of vaccine preventable diseases. The districts suggested by states have also been included. Considering the recent upsurge of COVID-19 cases, states have been given the flexibility of carrying out the activity either from February 2022- April 2022 or from March to May 2022. The first round will start from 7th February 2022 onwards, the second will be from 7th March 2022, and the third round will be from 4th April 2022. Unlike the past, each round will be conducted for seven days, including RI days, Sundays, and public holidays. However, considering the recent peak in COVID cases, States have been accorded the flexibility of conducting the drives from Mach to May 2022. 11 of the 33 states have planned to go ahead with the February – April 2022 schedule.
Shri Rajesh Bhushan, Union Health Secretary, Shri Vikas Sheel, AS&MD, Shri Lav Agarwal, Joint Secretary, Dr. P Ashok Babu, Joint Secretary, Dr. Harmeet Singh, Joint Secretary, Union Ministry of Health and Family Welfare and senior officials of the Ministry present in the event.
Under the aegis of ‘Azadi ka Amrit Mahotsav’, the Government has implemented two phases of awareness campaigns on HIV/AIDS, Tuberculosis and Voluntary Blood Donation. Phase II of awareness campaign on HIV/AIDS and TB was launched on 12th October 2021. The campaign endeavours to generate awareness regarding prevention of HIV/AIDS and TB, promotion of related services and reduce stigma and discrimination related to HIV/AIDS and TB.
During Phase I of the campaign, students from 834 schools and 889 colleges across the country were covered, including 25 schools and 100 colleges in the States of Maharashtra and Tamil Nadu. During the campaign, the students participated in various competitions like painting, online quiz, poster making, signature campaigns, mask making and reel making competitions to generate awareness on HIV/AIDS and TB.
The National AIDS Control Programme (NACP) is implemented by National AIDS Control Organisation (NACO) through State AIDS Control Societies (SACS) by allocating funds to them as grants-in-aid for providing HIV prevention, testing and treatment services. The States including Maharashtra and Tamil Nadu conducted the ‘Azadi ka Amrit Mahotsav’ campaign from grants-in-aid allocated to them for the year 2021-2022.
The awareness campaigns are a continuous process and regular activities are conducted in schools and colleges. Government of India launched National AIDS Control Programme (NACP) to address the HIV/AIDS disease in the country. NACP’s goal is to reduce annual new HIV infections and AIDS-related death by 80% since the baseline value of 2010 and the annual new HIV infections have declined by 48%. The achievement is 82% decline in AIDS-related death.
The key challenges faced in combating HIV/AIDS are stigma and discrimination.
SACS are implementing Adolescence Education Programme in Schools and Red Ribbon Club Programme in Colleges to raise awareness about HIV/AIDS and Out of School Youth programme in community to engage youth for awareness generation.
The Government of India is implementing a National Strategic Plan (NSP) for Tuberculosis (2017-2025) with the goal of achieving the SDG targets related to TB by 2025, five years ahead of the global target. The key strategies implemented under the National TB Elimination Programme (NTEP) are:
• Early diagnosis of all the TB patients, prompt treatment with quality assured drugs and treatment regimens along with suitable patient support systems to promote adherence
• Private sector engagement
• Prevention strategies including active case finding and contact tracing in high risk / vulnerable population
• Airborne infection control
• Multi-sectoral response for addressing social determinants related to TB
• Community engagement for a community led response
• Nutritional support through Nikshay Poshan Yojana
As per the Global TB Report 2021 by the World Health Organisation, the incidence rate for Tuberculosis in India has reduced from 217/lakh population in 2015 to 188/lakh population in 2020.
The key challenges in fighting Tuberculosis are raising the awareness levels of the community, improving health seeking behaviour of the population and addressing the social determinants of TB.
To raise awareness about TB among youth and adolescents, the National TB Elimination Programme has collaborated with Rashtriya Bal Swasthya Karyakram / Rashtriya Kishor Shakti Karyakram / Red Ribbon Clubs under NACP. Referral linkages for diagnosis and treatment of TB have been established with these programmes.
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Lok Sabha today.
National Institute of Pharmaceutical Education and Research (NIPER) Act was enacted in the year 1998 for setting up of an individual institute of national importance, viz., NIPER at SAS Nagar (Mohali), Punjab. The Act was subsequently amended in the year 2007 permitting establishment of similar institutes in different parts of the country. Six new NIPERs at Ahmedabad, Guwahati, Hyderabad, Kolkata, Raebareli and Hajipur were accordingly set up in 2007-08. In December, 2021, the Parliament has passed NIPER (Amendment) Bill, 2021 clarifying amongst others, that existing NIPERs and similar institutes set up subsequently would be institutes of national importance
NIPER at Mohali has a full-fledged campus with state of art laboratories and regular faculty. As regard six other NIPERs set up during 2007-08, the department has provided more than Rs. 1,200 cr. since their inception for their infrastructure and activities. These six NIPERs have since been sanctioned regular faculty and other administrative posts, most of which have been filled up. All these NIPERs have been provided funds for setting up of well-equipped laboratories. The construction of campus of NIPER at Guwahati has almost been completed and construction of campus of NIPER at Ahmedabad is in full swing. Expenditure Finance Committee (EFC) in its meeting held on 24th September, 2021 has further approved Rs. 1,500 cr. for the five-year period from 2021-22 to 2025-26 for setting up/ up-gradation of existing seven NIPERs, including construction of their regular campuses.
Expenditure Finance Committee in its last meeting has not supported proposal for creation of new NIPERs at present stage.
The information was given by the Union Minister of Chemicals and Fertilizers, Shri Mansukh Mandaviya in a written reply in the Lok Sabha today.
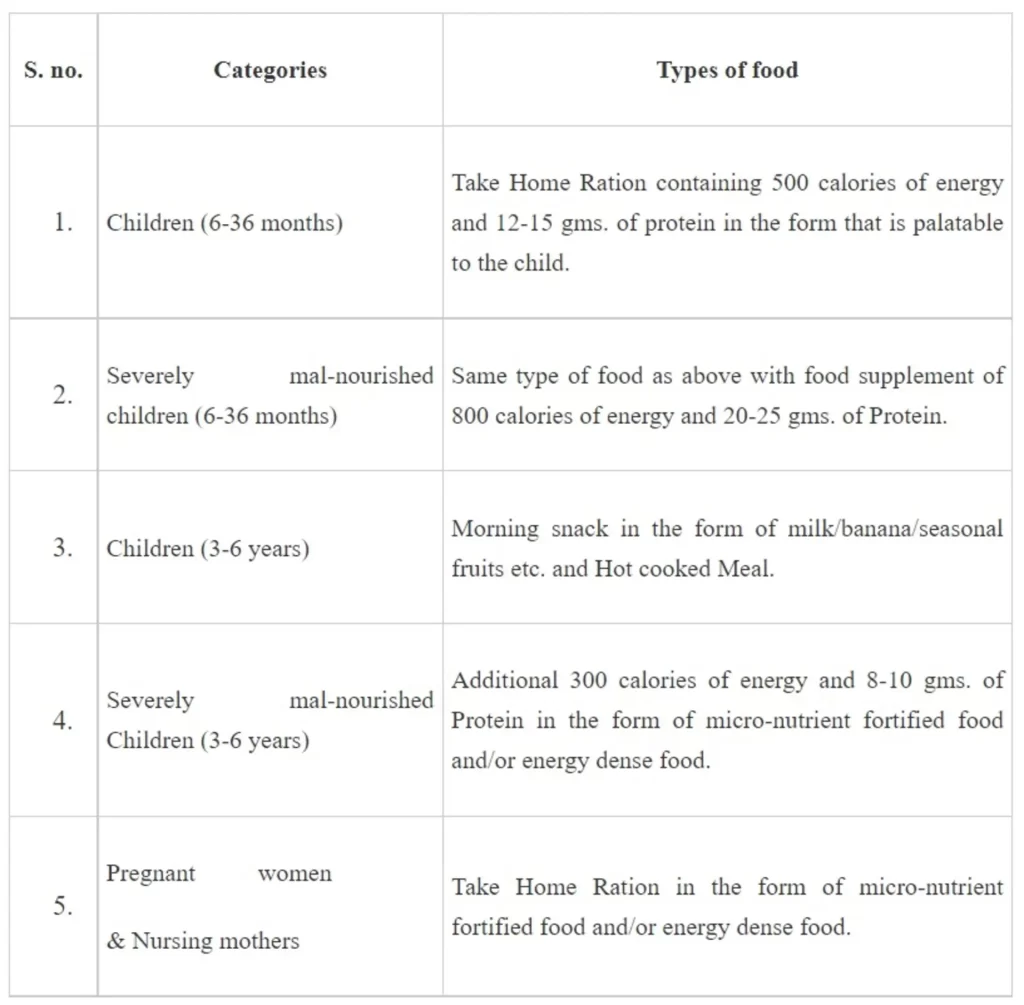
In 2018, the Government of India launched the Anaemia Mukt Bharat (AMB) strategy with the target to reduce anaemia in the vulnerable age groups such as women, children and adolescents in life cycle approach providing preventive and curative mechanisms through a 6X6X6 strategy including six target beneficiaries, six interventions and six institutional mechanisms for all stakeholders to implement the strategy. Under AMB strategy, the interventions for tackling the problem of anaemia in all the States and UTs include:
Prophylactic Iron and Folic Acid Supplementation in all six target age groups
Intensified year-round Behaviour Change Communication (BCC) Campaign for:(a) improving compliance to Iron Folic Acid supplementation and deworming, (b) enhancing appropriate infant and young child feeding practices, (c) encouraging increase in intake of iron-rich food through diet diversity/quantity/frequency and/or fortified foods with focus on harnessing locally available resources, and (d) ensuring delayed cord clamping after delivery (by 3 minutes) in health facilities
Testing and treatment of anaemia, using digital methods and point of care treatment, with special focus on pregnant women and school-going adolescents Addressing non-nutritional causes of anaemia in endemic pockets with special focus on malaria, hemoglobinopathies and fluorosis
Management of severe anaemia in pregnant women undertaken by administration of IV Iron Sucrose/Blood transfusion
Providing incentives to the ANM for identification and follow-up of pregnant women with severe anaemia in high priority districts (HPDs)
Training and orientation of Medical Officers and front line-workers on newer Maternal Health and Anaemia Mukt Bharat guidelines
Field level awareness by ASHAs through community mobilization activities and IEC and BCC activities
The prevalence of anaemia among six groups as per the National Family Health Survey 5 (2019-21), is 25.0 percent in men (15-49 years) and 57.0 percent in women (15-49 years). 31.1 percent in adolescent boys (15-19 yrs), 59.1 percent in adolescent girls,52.2 percent in pregnant women (15-49 years) and 67.1percent in children (6-59 months).
FewStates/UTs have shown decline in anaemia prevalence, details on theState/UT-wiseprevalenceof anaemia among six identified population groupsare placed at annexure.
The measures taken by the Government to make AMB programme more effective are:
working with other line departments and ministries for strengthening implementation
engaging National Centre of Excellence and Advanced Research on Anaemia Control (NCEAR-A) at AIIMS, Delhi in capacity building of health care providers strengthening supply chain and logistics
development of AMB Training Toolkit for capacity building of health care providers in anaemia management and recent launch of Anaemia Mukt Bharat e-Training Modules to facilitate training of the health care providers through virtual platform amid COVID 19 pandemic which has posed a challenge in capacity building through physical trainings.
Health is a State subject and the primary responsibility for strengthening health care services including implementation of national programs lies with the respective State/UT government. However, Government is taking steps to improve the condition of anaemia among all identified groups in all States/UTs. Ministry of Health and Family Welfare provides financial and technical support to States/UTs under NHM as proposed during annual Programme Implementation Plan. Covid-19 pandemic has also hampered AMB programme implementation contributing to anaemia prevalence among all the age groups
Annexure
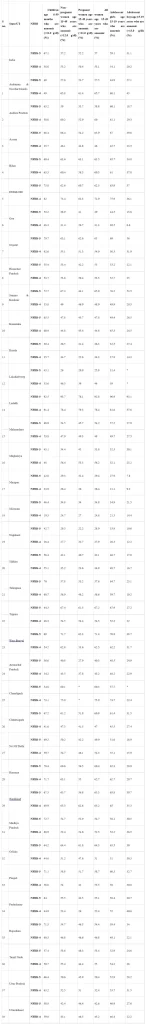
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Lok Sabha today.
The Ministry of Health & Family Welfare administers a Centrally Sponsored Scheme (CSS) for ‘Establishment of new Medical Colleges attached with existing district/referral hospitals’ with preference to underserved areas and aspirational districts, where there is no existing Government or private medical college. Under the Scheme, 157 new medical colleges have been approved in three phases and 70 are already functional. Out of 157 sites, 40 are in aspirational districts. The details are at Annexure.
Under Phase-III of the above Centrally Sponsored Scheme, all States/UTs were requested to submit proposals along with Detailed Project Report (DPR). No proposal was received from the State Government of Odisha for establishment of a medical college at Dhenkanal district.
Annexure
Details of medical colleges approved in aspirational districts under Centrally Sponsored Scheme for ‘Establishment of new Medical Colleges attached with existing District/Referral Hospitals’
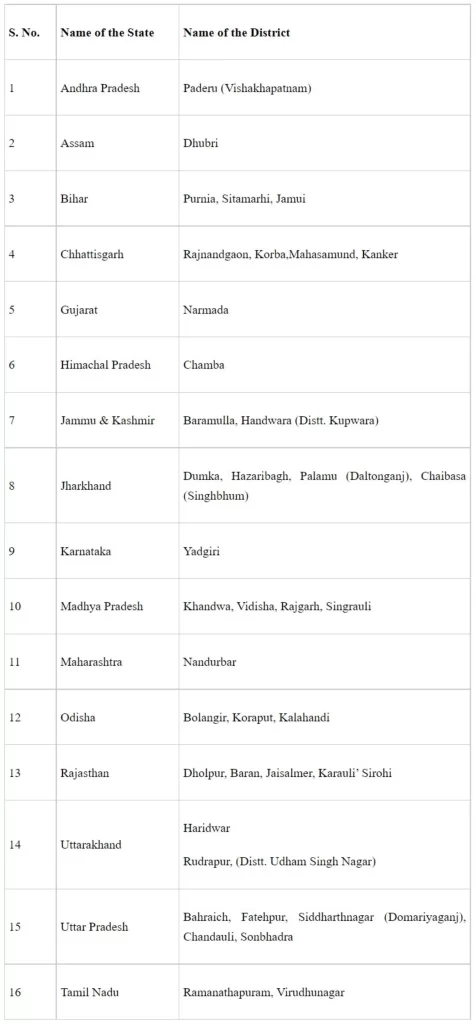
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Lok Sabha today.
The extant National Pharmaceutical Pricing Policy (NPPP), notified on 7th December, 2012, has been formulated with an objective to put in place a regulatory framework for pricing of drugs so as to ensure availability of essential medicines at reasonable prices while providing sufficient opportunity for innovation and competition to support the growth of pharma industry. The policy made a shift from earlier ‘cost based’ pricing under the Drug Policy, 1994 to ‘market based’ pricing.
In pursuance of NPPP, 2012, the Government notified the Drugs (Prices Control) Order, 2013 (DPCO-2013). As per the provisions of DPCO, 2013, the ceiling price of all scheduled formulations appearing in National List of Essential Medicines (NLEM), are fixed by National Pharmaceutical Pricing Authority (NPPA) and are uniform throughout the country. All the manufacturers of these drugs are required to sell their product equal to or lower than the ceiling price. Further, NPPA monitors the prices of non-scheduled drugs so as to ensure that the increase in their Maximum Retail Price (MRP) is not more than 10% of what was prevalent during preceding twelve months.
The information was given by the Union Minister of Chemicals and Fertilizers, Shri Mansukh Mandaviya in a written reply in the Lok Sabha today.
