A study ‘The burden of chronic respiratory diseases and their heterogeneity across the states of India: The Global Burden of Disease Study 1990-2016” was published in Lancet 2018 by ICMR. As per the study, the prevalence of Asthma reduced from 3468 per 100000 in 1990 to 3336 per 100000 in 2016 showing a decline of 3.8 percent over a period of 26 years.
Health is a state subject. The Department of Health & Family Welfare, however, provides technical and financial support to the States/UTs under the National Programme for Prevention and Control of Cancer, Diabetes, Cardiovascular Diseases and Stroke (NPCDCS), as part of National Health Mission (NHM), based on the proposals received in Program Implementation Plans (PIPs) from the States/UTs and subject to the resource envelope. The programme focusses on strengthening infrastructure, human resource development, health promotion & awareness generation for prevention, early diagnosis, management and referral to an appropriate level of healthcare facility for treatment of the given Non-Communicable Diseases including Chronic Obstructive Pulmonary Diseases (COPD) and Asthma.
Under NPCDCS, 640 NCD Clinics at District level and 5148 NCD Clinics at Community Health Centre level have been set up to ensure the treatment of common NCDs including Chronic Obstructive Pulmonary Diseases (COPD) and Asthma.
Patients with Acute Respiratory Infections (ARI), Chronic Obstructive Pulmonary Diseases (COPD) and Asthma are diagnosed and treated at various tertiary health care facilities such as Medical Colleges, Central Institutes like AIIMS, etc. The treatment in Government health facilities is either free, or highly subsidized for the poor and needy. The treatment for in-patient care is also available under Ayushman Bharat - Pradhan Mantri Jan Arogya Yojana (PMJAY) for 10.74 crore families eligible under AB-PMJAY as per Socio Economic Caste Census (SECC) database.
Under Free Drugs Service Initiative of NHM, financial support is provided to States/UTs for provision of free essential medicines. Furthermore, quality generic medicines are being made available at affordable prices to all, under Pradhan Mantri Bhartiya JanaushadhiPariyojana in collaboration with the State Governments.
Preventive aspect of NCDs including Chronic Obstructive Pulmonary Diseases (COPD) and Asthma is being strengthened under Comprehensive Primary Health Care under Ayushman Bharat - Health and Wellness Centers, by promotion of wellness activities and targeted communication at the community level. NPCDCS gives financial support under NHM for awareness generation (IEC) activities to be undertaken by the States/UTs as per their Programme Implementation Plans (PIPs), subject to resource envelope.
Further, in order to accelerate actions for reducing deaths due to Childhood Pneumonia (ARI), an initiative named “Social Awareness and Actions to Neutralize Pneumonia Successfully (SAANS)” has been launched in 2019 under Reproductive, Maternal, Newborn, Child and Adolescent Health (RMNCH+A) program under the aegis of NHM.
National Centre for Disease Control (NCDC) has also prepared and shared Information, Education and Communication (IEC) materials on Air Pollution as a risk factor for ARI, Chronic Obstructive Pulmonary Diseases (COPD) and Asthma, and shared it with all the States/UTs.
The Minister of State (The Ministry of Health and Family Welfare), Dr. BhartiPravin Pawar stated this in a written reply in the Lok Sabha here today.
Ayushman Bharat Pradhan Mantri Jan Arogya Yojana (AB PM-JAY) is a flagship health assurance scheme of the Government of India which aims at providing a health cover of Rs. 5 Lakhs per family per year for secondary and tertiary care hospitalizations for 10.75 Crore beneficiary families identified from Socio Economic and Caste Census (SECC) 2011 as per select deprivation and occupational criteria in rural and urban areas respectively. The scheme is currently being implemented by 33 State/UTs except West Bengal, Odisha and NCT of Delhi. These State/UTs have further expanded the beneficiary base to nearly 13.44 Crore families.
• Women make up 48.56% of eligible beneficiaries under AB PM-JAY as per SECC 2011 database.
• The health benefits packages under AB PM-JAY covers 1,669 procedures across 26 different specialties. Of these, 5 procedures deal exclusively with high-risk delivery.
For pregnant women specifically, the Janani Shishu Suraksha Karyakaram (JSSK)was launched with the objective to eliminate out of pocket expenses for both pregnant women and sick infants accessing public health institution and entitles them to free delivery, including caesarean section, free transport, diagnostics, medicines, other consumables, diet and blood in public health institutions.
Janani Suraksha Yojana (JSY), a safe motherhood intervention with the objective to reduce maternal and neonatal mortality by promoting institutional delivery among pregnant women especially with weak socio-economic status, i.e. women from SC/ST/BPL households is presently under implementation in all States/UTs with a special focus on Low Performing States and provides Cash incentives for women with the special focus for BPL/SC/ST women for institutional delivery (in government/ private accredited health facilities) and for BPL women who prefer for home delivery.
Other major initiatives supported under NHM are implementation of Free Drugs and Free Diagnostics Service Initiatives, PM National Dialysis Programme and implementation of National Quality Assurance Framework in all public health facilities including in rural areas. Mobile Medical Units (MMUs) & Telemedicine are also being implemented with NHM support to improve healthcare access particularly in rural areas.
As part of Ayushman Bharat, more than 77000Health and Wellness Centres (AB-HWCs) are operational across the country for provision of Comprehensive Primary Health Care (CPHC) that includes preventive healthcare and health promotion at the community level including screening of women for common non-communicable diseases.
Furthermore, States/UTs are being provided required technical and financial assistance for strengthening of their healthcare system including management of the COVID-19 public health challenge from time to time.
Further, to ensure that essential health services including treatment for non-COVID patients should not suffer, MoHFW has issued following guidelines and advisories for States/UTs:
Guidance note for enabling Delivery of Essential Health Services during the COVID 19 Outbreak on 14thApril, 2020.
Guidance note was issued on 21st May, 2020 for Immunization services.
Guidance note on Essential Reproductive, Maternal, Newborn, Child. Adolescent Health Plus Nutrition (RMNCAH+N) Services during and post COVID was issued on 27th May, 2020.
Advisory issued to ensure access to safe delivery and antenatal and postnatal care dated 16th June 2021.
The funds allocated under NHM for various Maternal Health Initiatives for FY 20-21 is Rs 2,233.48 Cr.
The funds allocated under NHM for RCH Flexipool for FY 20-21 is Rs 6,241.02(RE).
(d) & (e): “Public Health and Hospitals” being a State subject, the primary responsibility of strengthening public healthcare system, including ensuring provision of essential services including for pregnant women during the Pandemic, lies with the respective State Governments. However, the Ministry of Health and Family Welfare provides the technical and financial support to the States/UTs to strengthen the public healthcare system towards the objective of providing accessible, affordable and quality healthcare to all those who access public health facilities.
Under NHM, Mother and Child health (MCH) wings are established in District Hospitals/ District Women's Hospitals/ Sub- District Hospitals/CHC- First Referral Units (FRUs) to overcome the constraints of increasing caseloads and institutional deliveries at these facilities. More than 600 MCH wings have been sanctioned in the country.
NHM support is also provided for provision of a host of free services in public healthcare facilities in rural and backward areas including treatment of women specific diseases.
Support under National Health Mission (NHM) is provided to States/ UTs to supplement the efforts of the State/UT governments, including for setting up of new facilities as per norms and upgradation of existing facilities for bridging the infrastructure gaps, including in rural and backward areas and implementing national programme to provide quality healthcare in the public healthcare system, based on the requirements posted by them in their Programme Implementation Plans (PIPs) and within their overall resource envelope.
The Minister of State (The Ministry of Health and Family Welfare), Dr. Bharti Pravin Pawar stated this in a written reply in the Lok Sabha here today.
Central Government Health Scheme (CGHS) is a contributory health scheme primarily meant for Central Government Employees and Pensioners and their eligible family members, which provides primary healthcare through its Wellness Centres. Though, no CGHS Wellness Centre/ Hospital has been converted into a dedicated COVID Centre, however, CGHS has taken the following steps to contain the spread of COVID -19:-
(i) Medical Officers and staff were deployed at Airports for screening and for monitoring the international travelers isolated at Quarantine centres.
(ii) CGHS Wellness Centres operated ‘Fever Clinic’ for screening CGHS beneficiaries with complaints of fever and symptoms suggestive of COVID infection.
(iii) CGHS Medical Officers provided consultation and advice over telephone for COVID-19 positive CGHS beneficiaries, who had been advised home care.
(iv) CGHS Wellness Centreswere offered to State Governments to function as COVID-19 Vaccination Centres as per their suitability.
Due to superannuation, death, Voluntary retirement etc. of doctors and other staff, some posts in CGHS remain vacant.In order to ensure that the healthcare facilities to CGHS beneficiaries are not impacted, contractual Staff including services of retired Doctors and other staff are engaged against vacant posts as an interim measure till the posts are filled up on regular basis.
Improvement of CGHS facilities is a continuous dynamic process. Some of the initiatives taken during last few years under CGHS for the benefit of CGHS beneficiaries are as follows.
Expansion of CGHS coverage from 25 Cities in 2014 to 74 as on date
Simplification of referral system under CGHS
Facility for printing CGHS Card by the beneficiary
Provision for OPD consultation from Specialists of CGHS empanelled hospital after referral from CGHS Wellness Centre / CGHS Specialist
Direct Consultation from Specialists at empanelled hospitals in respect of elderly CGHS beneficiaries aged 75 years and above
Post-operative treatment in respect of critically ill beneficiaries is simplified and one-time permission without the need for revalidation from time to time. The consultation /investigations are permitted under these follow-up cases. The conditions covered are:
Post Cardiac Surgery Cases including Coronary Angioplasty
Post Organ Transplant Cases (Liver, Kidney, Heart, etc.,)
Post Neuro Surgery Cases/Post Brain Stroke cases requiring regular follow-up treatment
End Stage Renal Disease/follow up cases of Liver Failure
Cancer treatment
Auto-immune disorders like Rheumatoid Arthritis requiring regular follow-up
Neurological disorders like Dementia, Alzheimer’s disease, Parkinsonism, etc.,
Helpline for information and for lodging Complaints.
Aadhar based Attendance system at CGHS Wellness Centres for punctuality
Online appointment for consultation with Medical Officers at CGHS, Wellness Centres. Online transfer of CGHS card on account of transfer from one CGHS covered city to another CGHS covered City in respect of serving employees also.
Paperless settlement of Hospital Bills by CGHS through NHA-IT Platform w.e.f. 01.06.2021
Online process for payment of CGHS subscription by pensioners on the Bharatkosh platform.
To facilitate consultation with specialists through virtual mode, CGHS has started tele-consultation services for its beneficiaries through e-Sanjeevani portal.
Fortnightly webinars on relevant health topics are conducted.
Approval of Department of Expenditure, Ministry of Finance for creation of posts to man 16 new Wellness Centres, which include new cities like Panchkula, Mysuru, Nasik, Aurangabad, Chandrapur, Coimbatore has been obtained.
The Minister of State (The Ministry of Health and Family Welfare), Dr. Bharti Pravin Pawar stated this in a written reply in the Lok Sabha here today.
“Public Health and Hospitals” being a state subject, the primary responsibility of strengthening public healthcare system, including for provision of quality healthcare and advanced treatment and diagnostic facilities, lies with the respective State Governments. However, the Ministry of Health and Family Welfare provides technical and financial support is provided to the States/UTs to strengthen the public healthcare delivery at public healthcare facilities.
Under the National Health Mission (NHM), financial and technical support is provided to States/UTs to strengthen their health care systems including setting-up/upgrading public health facilities and augmenting health human resource on contractual basis for provision of equitable, affordable and quality healthcare with modern treatment methods and diagnostic facilities in the public healthcare facilities of the Country including rural areas based on requirements posed by the States in their Programme Implementation Plans (PIPs).
NHM support is also provided for provision of a range of free services related to maternal health, child health, adolescent health, family planning, universal immunisation programme, and for major diseases such as Tuberculosis, vector borne diseases like Malaria, Dengue and Kala Azar, Leprosy etc.
Other major initiatives supported under NHM include Janani Shishu Suraksha Karyakram (JSSK) (under which free drugs, free diagnostics, free blood and diet, free transport from home to institution, between facilities in case of a referral and drop back home is provided), Rashtriya Bal Swasthya Karyakram (RBSK) (which provides newborn and child health screening and early interventions services free of cost for birth defects, diseases, deficiencies and developmental delays to improve the quality of survival), implementation of Free Drugs and Free Diagnostics Service Initiatives, PM National Dialysis Programme and implementation of National Quality Assurance Framework in all public health facilities including in rural areas.
Mobile Medical Units (MMUs) & Tele-consultation services are also being implemented to improve access to healthcare particularly in rural areas.
As part of Ayushman Bharat, the Government is supporting the States for transformation of Sub Health Centres and Primary Health Centres into 1.5 lakh Health and Wellness Centres across the country by December, 2022 for provision of Comprehensive Primary Health Care (CPHC) that includes preventive healthcare and health promotion at the community level with continuum of care approach. Under this programme, CPHC services of an expanded range of services, that are universal and free to users, with a focus on wellness, are provided, closer to the community. Further Ayushman Bharat, Pradhan Mantri Jan Arogya Yojana (AB-PMJAY) provides health coverage up to Rs 5 Lakh per family per year to around 10.74 crore poor and vulnerable families as per Socio Economic Caste Census (SECC).
Financial support is also provided to States for providing hard area allowance, performance-based incentives, providing accommodation and transport facilities in rural and remote areas including tribal areas, sponsoring training programmes, etc to engaged human resources to address the issue of shortage of doctors and specialists in the public health facilities.
In the 15 years of implementation, the NHM has enabled achievement of the Millennium Development Goals (MDGs) for health. It has also led to significant improvements in maternal, new-born, and child health indicators, particularly for maternal mortality ratio, infant and under five mortality rates, wherein the rates of decline in India are much higher than the global averages and these declines have accelerated during the period of implementation of NHM.
Report of NITI Aayog (March 2021), collated the three Studies done on the aspects of Governance, Human Resources, Financing and Health outcomes and the key findings of the Report are as follows:
There has been significant improvement in the infrastructure facilities during NHM period with an increase in number of beds in the government hospitals as well in the community health centers (CHCs) from 0.44 in 2005 to 0.7 in 2019 per 1000 population. The focus on infrastructure improvement resulted in construction of more than 46,000 health facilities, with a significant increase in the total number of first referral units (FRUs) (940 in 2005 to 3057 in 2019).
The number of doctors, nurses in PHCs and CHCs also increased during the NHM periods. An additional 200,000 healthcare providers (from auxiliary nurse-midwives (ANMs) to specialists’ doctors) and 850,000 village level ASHA in rural areas were recruited during the NHM period.
There is strong evidence to show that increased infrastructure and increased human resources has had a positive effect on improving the availability, affordability and accessibility of maternal and child services, leading to improved antenatal and postnatal care and improved maternal and child outcomes.
Maternal and child indicators such as the IMR, NMR and MMR have shown a marked improvement in the NHM period. There has been a remarkable decline in under five mortality rate (U5MR) from 78 to 37 per thousand live births from 2005 to 2019. The infant mortality rate (IMR) declined from 58 per 1000 live births to 32 per 1000 live births during 2013-18. the neonatal mortality reduced from 38 per thousand live births to 22 per thousand live births, with a percentage decline of 42.1% from 2005 to 2019. Maternal mortality ratio (MMR) declined by 52%, from 257 per lakh live births in 2004-06 to 122 per lakh live births, in 2015-17.
Improvements in maternal and child indicators can be attributed to better implementation of facility based newborn care including sick newborn care units (SNCUs), evidenced from systematic review.
Various studies showed that Janani Suraksha Yojana (JSY) strategy had a strong evidence in promoting institutional delivery and reducing perinatal mortality. JSSK had a role in providing free diagnostics by improving the affordability.
There is strong evidence that shows that child health strategies such as Facility Based Newborn Care (FBNC), Home Based Post Natal Care (HBPNC), Integrated Management of Neonatal and Childhood Illness (IMNCI) and immunization improved the availability, affordability and accessibility of child health services especially for the rural and poor community.
There has been steady decline in out-of-pocket expenditure for under five child hospitalization, institutional deliveries and catastrophic hospitalizations as per consecutive rounds of NSS surveys. Multiple schemes launched by the government like free transport, free diagnostics, free dialysis, and free drug / Jan AushadhiKendras are initiatives that have contributed to reducing OOPE.
The Minister of State (The Ministry of Health and Family Welfare), Dr. Bharti Pravin Pawar stated this in a written reply in the Lok Sabha here today.
Union Ministry of Health and Family Welfare in partnership with UNICEF, today, hosted an interactive communication session for representatives of Community Radio Stations and Private Radio Stations for creating meaningful awareness campaigns surrounding various issues related to COVID including about adhering to COVID Appropriate Behaviour (CAB), benefits of vaccine and to dispel misinformation and myths.
The session was addressed by Shri Lav Agarwal, Joint Secretary, MoHFW and was attended by over 70 representatives of Community Radio Stations and Private Radio stations from the five states of southern India- Kerala, Karnataka, Telangana, Andhra Pradesh and Tamil Nadu.
Shri Lav Agarwal, in his key note address acknowledged the contribution of radio stations in supporting the world’s largest vaccination drive by airing educative programs for their listeners and inspiring stories of HealthCare Workers (HCWs) and community participation in spreading message to follow Covid Appropriate Behaviour. These efforts played a positive role in uptake of vaccination among large number of vaccine eligible population while mitigating any vaccine and vaccination rumours, he added.
He emphasized that radio stations are a critical medium in delivering COVID messages among population residing in urban as well as remote areas. He said that radio plays a constructive role through innovative and engaging programmes to address unfounded concerns of linked to vaccine hesitancy by inviting subject experts on their program.
He urged the participants to highlight community led positive initiatives and role models from the frontline workers across sectors to strengthen public trust in world’s largest adult vaccination programme. He also underlined the need to continuously remind citizens about need to strictly follow COVID Appropriate Behaviour as the second wave is still not over and that virus can come back as soon society ignores COVID safe behaviour.
He also emphasized on the importance of mental wellbeing during COVID and suggested that it is vital to address the issue on a regular basis. He further said that there are three important components of the fight against COVID - Community ownership of COVID Appropriate Behaviour, Evidence Based Reporting and Busting Myths on COVID and vaccination.
He presented a snapshot of the COVID situation in the country and highlighted the status of five states. He highlighted the various initiatives and steps being taken by the Government to strengthen the public health infrastructures.
The participants shared their experiences of innovative radio and talk shows to educate and inspire the listeners. Senior officials of the MoHFW, Ministry of Information & Broadcasting, and representatives from UNICEF attended the session.
On the advice of NITI Aayog, an external evaluation of National AIDS Control Programme (NACP) was conducted in 2020, which found that ‘programme has done a commendable job and performed very well’. NACP-IV and its extension phase (2012-21) largely achieved the goals and targets set out at the initiation of the phase. The external evaluation did not report any misuse of programme funds. Further, no such instance has come to the notice of the Government.
In the last three financial years viz., 2018-19, 2019-20 and 2020-21, the utilisation of fund under NACP has been 93.7%, 94.9% and 97.1% respectively. As a result of sustained efforts being made under this Programme of the Government of India, HIV epidemic in India continues to be low nationally, with an estimated adult (15-49 yrs.) prevalence of 0.22% in 2020. Estimated annual new HIV infections in the country have declined by 48% (between 2010 and 2020) in comparison to the global average of 31%. Estimated annual AIDS-related mortalities have declined by 82% (between 2010 and 2020) in comparison to the global average of 42%.
The Minister of State (The Ministry of Health and Family Welfare), Dr. Bharti Pravin Pawar stated this in a written reply in the Rajya Sabha here today.
Ministry of Health & Family Welfare has advised States/UTs to undertake various initiatives to recognize services rendered by healthcare workers engaged in COVID-19 related duties. Some of these include:
All such professionals who sign up for minimum 100 days of Covid duty and complete it successfully will be given the Prime Minister’s Distinguished Covid National Service Samman from Government of India.
State/UT Governments to consider giving preference in regular Government appointments of Health professionals through the respective Public Service Commission/ other recruitment bodies, for those Health Professionals under this special scheme, who complete a minimum of 100 days of Covid related duty.
States/UTs may also consider giving suitable honorarium for distinguished Covid Service as per NHM norms.
Government of India has introduced a new category called ‘Wards of COVID Warriors’ in the guidelines for selection and nomination of candidates against Central pool MBBS seats for the academic year 2020-21. Five Central pool MBBS seats were reserved for this category for the academic year 2020-21. MBBS seats were allocated for Central pool MBBS seats for candidates from amongst the wards of “COVID Warriors”, who have lost life due to COVID 19; or died accidently on account of COVID 19 related duty.
Further, realizing the criticality of human resources at the time of pandemic, Ministry of Health & Family Welfare has taken a number of steps to improve wellbeing of healthcare workers. Few of the actions taken in this regard include:
With the launch of COVID-19 vaccination initiative on 16th January 2021, Healthcare workers were identified as one of the first priority group. State Governments/ UT administrations have been repeatedly urged to ensure that the medical professionals engaged in Covid related work are suitably vaccinated.
Ministry of Health and Family Welfare provided guidelines on Infection Prevention and Control practices to the State Governments to minimize the risk of infection to healthcare workers.
To build the capacities of human resources including the medical personnel, non-medical personnel and front-line workers for COVID-19 management an ‘Advisory for Human Resource Management of COVID-19’ was issued to provide guidance to States/UTs on the human resources mobilization, their role assignment and training requirements for COVID-19 management.
The training resources for medical and non-medical personnel on infection prevention and control, clinical management including ventilation, logistics etc. is being updated regularly and is available on the website of Ministry of Health & Family Welfare.
Online training and webinars for physicians and nursing personnel have been conducted by AIIMS on management of patients with COVID-19, septic shock, ventilation strategy, management of aerosol generating medical procedures, infection and prevention control practices, psychological care of patients etc.
In addition, training modules have also been made available on iGOT online platform by DOPT (https://igot.gov.in/igot). These include:
Basics of COVID-19
Quarantine and isolation
Infection prevention through PPE
Psychological care of patients with COVID-19
Infection prevention and control
Laboratory sample collection and testing
Clinical management of COVID-19
Management of COVID-19
ICU Care and Ventilation Management
Capacity building initiatives to conduct large scale containment operations for active case search and tracking has been carried out through training of State Surveillance Officers, Rapid Response Teams and grass root level workers/volunteers identified for surveillance activities, ASHAs, Anganwadi Workers, Auxiliary Nurse Midwives, National Service Scheme, Indian Red Cross Society volunteers, Nehru Yuvak Kendra Volunteers, Ayush Students and National Cadet Corps.
A Clinical Center of Excellence (CoE) initiative has also been launched by Union Ministry of Health with AIIMS, Delhi as apex nodal institution and State level CoEs to provide guidance on clinical management protocols. AIIMS, Delhi is conducting regular webinars on clinical management and related aspects and the State CoEs are further disseminating it to their medical colleges, district and sub-district hospitals.
The Minister of State (The Ministry of Health and Family Welfare), Dr. Bharti Pravin Pawar stated this in a written reply in the Rajya Sabha here today.
Indian Council of Medical Research (ICMR), an autonomous body under the Department of Health Research, has established a COVID clinical registry at 20 sites across the country to capture clinical treatment and outcomes of COVID-19. This information is only limited to hospitalized patients. Post Covid studies are being carried out on various conditions like aortic and lung inflammation, mucormycosis etc. Although, Health is a State subject, Government of India has advised the States to establish post COVID clinics in their respective appropriate health facilities to cater to the needs of people suffering various post COVID conditions.
Also, expert groups are working on modules/guidelines on various post COVID conditions/issues.
The Minister of State (The Ministry of Health and Family Welfare), Dr. Bharti Pravin Pawar stated this in a written reply in the Rajya Sabha here today.
The Government took various measures to increase the supply of essential drugs such as granting expeditious approvals to new manufacturing sites of existing manufacturers to enhance their production capacity, issuing licenses to new manufacturers/importers, helping the manufacturers in sourcing raw material and helping importers of drugs in getting maximum supplies on priority from the importing countries through support from diplomatic channels, restricting exports for a certain period, and allocating the drugs namely Remdesivir, Tocilizumab and Amphotericin B, during the period of limited supply, to States in an equitable manner to ensure availability of these drugs across the country. Domestic production and import of critical drugs was monitored regularly by the Government. Regular meetings were held with manufacturers to identify and address the issues faced by the manufacturers in the augmentation of the production. The availability of all major drugs required for management of COVID-19 was regularly monitored through weekly surveys of retail pharmacies.
Remdesivir is a patented drug of Gilead Life Sciences USA, manufactured in India under voluntary licenses granted by the patent holder to 7 Indian pharmaceutical companies. With the accelerated approval of 40 additional manufacturing sites by the Central Drugs Standard Control Organisation (CDSCO), the number of approved manufacturing sites has increased from 22 in mid-April, 2021 to 62 in June, 2021. The domestic production capacity of all the seven licensed manufacturers was thus augmented from 38 lakh vials per month in mid-April, 2021 to nearly 122 lakh vials per month in June, 2021. Total domestic production of Remdesivir by seven licensed manufacturers between 1st April and 25th July, 2021 is 1,68,14,752 vials.
Tocilizumab is a patented drug of Hoffman La Roche, a Swiss multinational company. It is not manufactured in India and is available in India through imports only. Its imported quantity was maximized through persistent efforts of the Government with the sole manufacturer of Tocilizumab. 1,00,020 vials (80 mg) and 13,001 vials (400mg) were commercially imported between 1st April and 25th July, 2021. In addition, 50,024 vials (80 mg) were received in donation from Roche in the month of May, 2021.
Department of Pharmaceuticals and the Drug Controller General of India (DCGI) actively coordinated with the industry for identification of manufacturers and expeditious approvals of new manufacturing facilities. The DCGI issued manufacturing/marketing permission of Amphotericin B Liposomal Injection to 11 new companies in the months of May and June, 2021. The domestic production of Liposomal Amphotericin B between 1st May and 30th June, 2021 is 4,53,555 vials. The expected production in the month of July, 2021 is 3,45,864 vials.
Department of Pharmaceuticals and the Indian Embassy in the USA worked continuously with importers and manufacturers to maximise the quantity of imports of Liposomal Amphotericin B and also for early delivery of supplies. The total import of Liposomal Amphotericin B between 1st May and 29th July, 2021 is 10,77,677 vials. Indian Missions all over the world were instructed to immediately identify additional sources of the Liposomal Amphotericin B. MEA also helped domestic manufacturers in getting supplies of key excipients viz. HSPC and DSPG-Na required for production of Liposomal Amphotericin B from sources abroad.
The domestic production and imports of other drugs required for the management of COVID-19 namely dexamethasone, methylprednisolone, paracetamol etc. was monitored regularly and there was sufficient availability of these drugs to meet the increased demand.
The allocation of Remdesivir, Tocilizumab and Amphotericin B was started on 21st April, 27th April and 11th May, 2021 respectively. The allocation of Remdesivir and Amphotericin B has now been discontinued due to sufficient availability of these medicines. The last allocation of Remdesivir was done on 23rd May, 2021 and that of Amphotericin B was done on 24th July, 2021. In addition to above commercial supplies, Central government has supplied to States free of cost Remdesivir, Tocilizumab and Amphotericin B received through Donation and also procured by the Central Government.
This information was given by the Minister of Health & Family Welfare and Chemicals & Fertilizers, Shri Mansukh Mandaviya in a written reply in Lok Sabha today.
The measures taken by Department of Commerce to promote exports include various schemes under the Foreign Trade Policy (FTP), assistance under the Market Access Initiative (MAI) scheme, setting up district export hubs, Transport and Market Assistance Scheme etc. Trade delegations/buyer-seller meets with various countries are regularly organized for the benefit of exporters. Airfare support is also provided to the exporters with a turnover of Rs.30crore and below to encourage participation in business delegations/trade fairs.
The quantum of pharmaceutical exports of past three years, category-wise is as under:
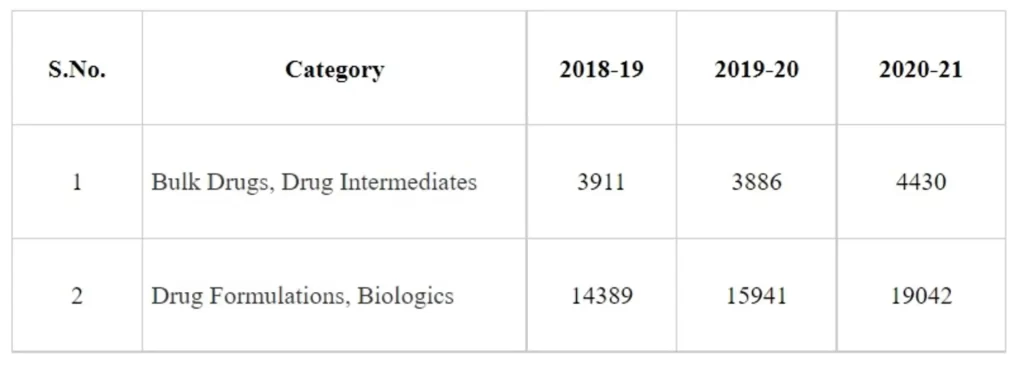
Department of Commerce, in partnership with other stakeholders, is working towards boosting our presence in under penetrated/potential international markets viz. North East Asia, Africa, Middle East, Latin America, South East Asia etc. The Department is also actively taking up with MoHFW/CDSCO for promotion of newer products such as gene therapy, bio-similars, and specialty drugs to drive the next phase of export growth.
This information was given by the Minister of Health & Family Welfare and Chemicals & Fertilizers, Shri Mansukh Mandaviya in a written reply in Lok Sabha today.
