India’s COVID-19 vaccination coverageexceeded 43.51 Cr yesterday. Cumulatively,43,51,96,001vaccine doses have been administered through 52,95,458sessions, as per the provisional report till 8 am today. 18,99,874vaccine doses were administered in the last 24 hours.
These include:
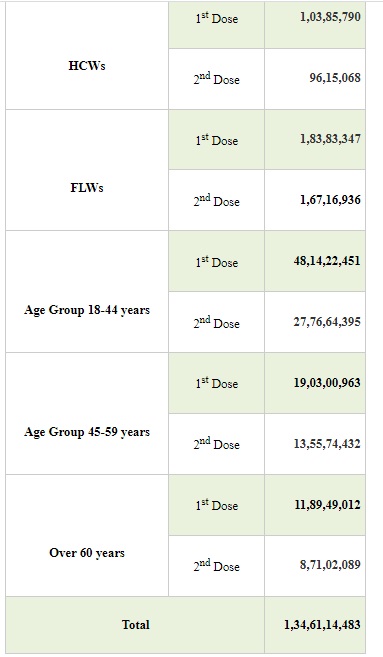
The new phase of universalization of COVID-19 vaccination has commenced from 21st June, 2021. The Union Government is committed to accelerating the pace and expanding the scope of COVID-19 vaccination throughout the country.
Out of the people infected since the beginning of the pandemic, 3,05,79,106people have already recovered from COVID-19 and35,968patients have recovered in the last 24 hours. This constitutes an overall recovery rate of 97.35%.
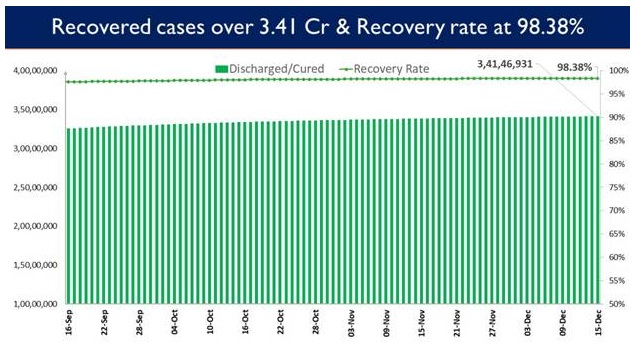
India has reported 39,361daily new cases in the last 24 hours.
Less than 50,000 Daily New Cases have been reported since twenty-nine continuous days. This is a result of sustained and collaborative efforts by the Centre and the States/UTs.

India’s Active Caseload today stands at 4,11,189and active cases now constitute1.31% of the country's total Positive Cases.
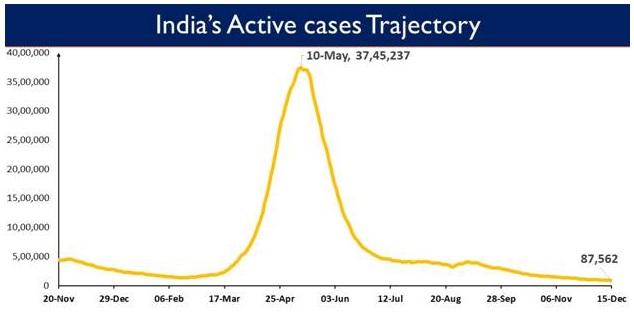
With substantially ramped up testing capacity across the country, a total of 11,54,444tests were conducted in the last 24 hours in the country. Cumulatively, India has conducted over 45.74 crore (45,74,44,011) tests so far.
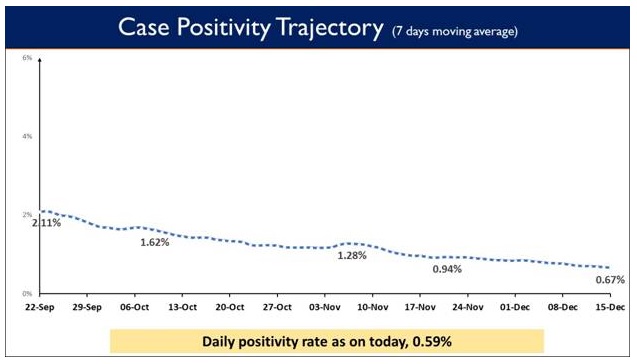
While on one side testing capacity has been enhanced across the country, Weekly Positivity Rate is currently at 2.31% and the Daily Positivity rate stands at 3.41% today. Daily Positivity rate has remained below 5%for 49 consecutive days now.
Dr Manju Puri, Head, Department, Obstetrics and Gynaecology, Lady Hardinge Medical College, New Delhi talks about the recent decision to administer Covid-19 vaccination during pregnancy, and what precautions women should take to protect herself and her child from catching COVID-19.
It has now been approved that woman can take COVID-19 vaccines even during pregnancy. How will it help?
During the second wave, many women contracted COVID-19 during pregnancy compared to the first wave. COVID if severe can lead to serious complications during pregnancy, especially during the last trimester as the uterus is enlarged and presses on the diaphragm, compromising a woman’s ability to cope with a fall in oxygen saturation. This may lead to a sudden fall in blood oxygen saturation and risk the lives of both the mother and the child. Vaccines will help prevent severe disease in pregnant women.
Also, vaccinating a mother is likely to give some degree of protection to the new-born as the antibodies developed in the mother’s body post-vaccination will pass on to the developing foetus through her blood. In the case of lactating mothers, an infant gets these antibodies through the mother’s breast milk.
Some people believe that vaccines can cause infertility among women. Is it true?
These are rumours that get circulated on ubiquitous social media. Misinformation is far more dangerous than virus itself.
Though the Covid-19 vaccines are relatively new, these have been developed using time tested techniques. Vaccines help the body develop immunity against a specific pathogen, it does not affect any other body tissue. In fact, we give some vaccines such as hepatitis B, Influenza, pertussis vaccine to women even during pregnancy to protect them and their unborn child from various diseases.
Besides, our regulators have approved the administration of the vaccines during pregnancy only after they were confident of their safety. There is no scientific data or studies that show that vaccines can cause infertility. These vaccines do not affect the reproductive organs in any way.
What precautions should a pregnant woman take to protect herself from catching COVID?
Pregnancy and childbirth are social events in our society. But during the pandemic, it may mean exposing the mother and child to infection. We recommend that an expectant mother should wear a mask and maintain physical distance even when at home, amongst her family members. It is because she may not be going out, but her family members could be going out for work and she can contract the infection from them.
So, women should use all Covid-Appropriate precautions during pregnancy, and after childbirth as it can prevent them from catching the infection and related complications.
What should a pregnant woman do if she shows symptoms of Covid-19?
First, if they have any symptoms of COVID, they should get themselves tested at the earliest, as the sooner we diagnose, the better we can manage the disease. The management of COVID is almost the same during the pregnancy as it is for others, but it should be done only under the strict supervision of a doctor.
A woman should isolate herself, drink plenty of fluids, check her temperature and oxygen saturation every 4-6 hrs. If the temperature does not come down even after taking paracetamol, she needs to contact the doctor; if there is a fall in oxygen concentration or if there is a decreasing trend for example if it is, say, 98 in the morning, 97 in the evening, and then drops further the next day, she needs to get in touch with her doctor.
Besides, women who have associated illnesses such as diabetes, high blood pressure, cardiovascular disease, obesity, etc, need to be more careful, as they may need hospitalisation. So, consult your doctor and keep in touch with your doctor throughout the recovery period.
We strongly recommend an overall health check-up post-Covid recovery to ensure that the mother and the foetus are doing fine.
Can a foetus contract Covid-19 from the mother?
There is no evidence to support this concern. We have done a couple of studies and found that the placenta, an organ that is formed in the uterus in which a foetus grows, acts as a protective barrier. There are a few cases where the new-born were found infected but we are not sure whether those babies got the infection inside the mother’s womb or soon after the birth.
Having said that, as I have explained earlier also, pregnant women must take all the possible precautions to prevent the infection as Covid-19 can affect her and her child in many other ways.
What precautions should a COVID positive mother take to protect her newborn?
A mother should continue to breastfeed the baby but is advised to keep the baby at a distance of 6 feet from her when she is not breastfeeding. A caregiver who is tested negative can also help in taking care of the newborn. Before breastfeeding the newborn, she should wash her hands, wear protective gear such as a mask, face shield. She should also sanitize her surroundings frequently.
If there is no one else to take care of the child, a mother should wear a mask all the time, and maintain physical distance from the child as much as possible. The mother and the child should stay in a well-ventilated room. And she should regularly wash her hands and sanitise the surroundings.
Postpartum depression and anxiety are common among women. Do you see an increase in mental health issues among women during the pandemic?
Certainly, there is an increase in mental health problems among women during pregnancy and post-childbirth. These are times when a woman undergoes a lot of hormonal and physiological changes. She has poor coping skills and needs social support. In the absence of this social support, she can feel lonely, helpless, and depressed.
Isolation for 15-days is difficult for everyone, but more so for pregnant women and postnatal mothers. During this time, the additional anxiety about her child’s health can severely affect her mental status.
So, it is important to provide constant support and assurance to women during this time. The family should stay in touch through video calls, and observe any change in her mood and seek medical help if she looks and feels depressed.
We always ask our pregnant women and mothers two simple screening questions: One, does she have little or no interest in doing her routine chores? And second, does she feel sad or feel like crying without any specific reason anytime in the past 2 weeks? If the answer is yes to any of these questions it means she needs further evaluation by a psychologist. Doctors, as well as family members, need to watch a woman’s behaviour carefully during this time.
What advice would you like to give to your women patients?
We ask them to stay safe, take adequate precautions and follow Covid-Appropriate Behaviour. Take vaccine as and when it is available to them. Avoid meeting many people.
If they have symptoms suggestive of COVID such as fever, sore throat, loss of taste or smell or exposure to a COVID positive person they need to seek medical help immediately, should not delay the diagnosis and should not self-treat. And lastly, we also counsel all our pregnant women about various contraceptive methods during pregnancy and offer them postpartum Intra-Uterine Device (Cu T), which can be inserted immediately after childbirth or caesarean delivery. It saves them of an unnecessary visit to the hospital after childbirth and reduces the risk of an unplanned pregnancy.
The Union Government of India, aware about the challenges posed by anti-microbial resistance (AMR) in the country, has taken following measures to address the issue:
National programme on AMR containment was launched during 12th FYP in 2012-17. Under this programme, AMR Surveillance Network has been strengthened by establishing labs in State Medical College. 30 sites in 24 states have been included in this network till 30th March 2021.
National Action Plan on Antimicrobial Resistance (NAP-AMR) focusing on One Health approach was launched on 19th April 2017 with the aim of involving various stakeholder ministries/departments. Delhi Declaration on AMR– an inter-ministerial consensus was signed by the ministers of the concerned ministries pledging their support in AMR containment. In the line with NAP-AMR three states have launched their state action plan
Kerala has launched KARSAP
Madhya Pradesh has launched MP-SAPCAR
Delhi has launched SAPCARD
AMR Surveillance Network: ICMR has established AMR surveillance and research network (AMRSN) in 2013, to generate evidence and capture trends and patterns of drug resistant infections in the country. This network comprises of 30 tertiary care hospitals, both private and government.
AMR Research & International Collaboration: ICMR has taken initiatives to develop new drugs /medicines through international collaborations in order to strengthen medical research in AMR.
ICMR along with Research Council of Norway (RCN) initiated a joint call for research in antimicrobial resistance in 2017.
ICMR along with Federal Ministry of Education and Research (BMBF), Germany has a joint Indo-German collaboration for research on AMR.
Initiatives to control overuse or misuse of antibiotics: ICMR has initiated antibiotic stewardship program (AMSP) on a pilot project basis in 20 tertiary care hospitals across India to control misuse and overuse of antibiotics in hospital wards and ICUs.
On the recommendations of ICMR, DCGI has banned 40 fixed dose combinations (FDCs) which were found inappropriate.
ICMR worked in collaboration with Indian Council of Agriculture Research, Department of Animal Husbandry, Dairy and Fisheries and the DCGI to ban use of Colistin as growth promoter in animal feed in poultry.
National Guidelines for Infection Prevention and Control in Healthcare Facilitieshave been released by MoHFW in Jan 2020. (https://ncdc.gov.in/showfile.php?lid=431)
ICMR has developed evidence based treatment guidelines for treatment of ten syndromes of infections. It aims to rationalize the usage of antibiotics on Essential Medicines Formulary (EMF) and to establish consistency in the treatment of various infectious conditions.
Further, ICMR has also issued the Treatment Guidelines for Antimicrobial Use in Common Syndromes” in 2019.
(https://www.icmr.nic.in/sites/default/files/guidelines/Treatment_Guidelines_2019_Final.pdf)
Media material has been developed to create awareness among various stakeholders regarding AMR and appropriate use of antibiotics.
Yes. Government is working on One Health approach by encouraging interdisciplinary collaboration at the human-animal-environmental interface.
The key priority areas include zoonotic diseases (emerging and re-emerging), food safety and antibiotic resistance.
Program for Strengthening Inter-sectoral Coordination for Prevention and Control of Zoonotic Diseases’ was launched in the 12th Five-year plan (2012-17) which is still continuing as “National One Health Program for Prevention and Control of Zoonoses” in 15th Finance Commission (2021-26) period.
This scheme aims to operationalize “One Health” Mechanisms for prevention and control of Zoonoses by strengthening inter-sectoral coordination among all stakeholders. In this regard, National Institute of One Health is being established at Nagpur which will house BSL IV laboratory.
ICMR has undertaken a project on an “Integrated One Health Surveillance Network for Antimicrobial Resistance” in collaboration with Indian Council of Agriculture research (ICAR) to assess the preparedness of Indian Veterinary laboratories to participate in integrated AMR surveillance network. ICMR has also created veterinary standard operating procedure (Vet-SOPs) for enabling comparison of antimicrobial resistance patterns in animals and humans. (https://main.icmr.nic.in/sites/default/files/guidelines/SOP_Bacteriology_Veterinary_2019.pdf)
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Lok Sabha here today.
In a significant decision by the Union Government, National Pharmaceutical Pricing Authority (NPPA) exercising extraordinary powers in public interest, has capped the Trade Margin vide notification dated 13th July 2021 for five Medical Devices.
These are:
Pulse Oximeter,
Blood Pressure Monitoring Machine,
Nebulizer,
Digital Thermometer, and
Glucometer.
The margin was capped up to 70% on Price to Distributor (PTD) level. Pursuant there to, a total of 684 products/brands of these medical devices have been reported as on 23rd July 2021 and 620 products/brands (91%) have reported downward revision of MRP.
The maximum downward revision has been reported by imported brand of Pulse Oximeter, showing reduction of Rs. 2,95,375 per unit. The details of price reduction are given in the table below:
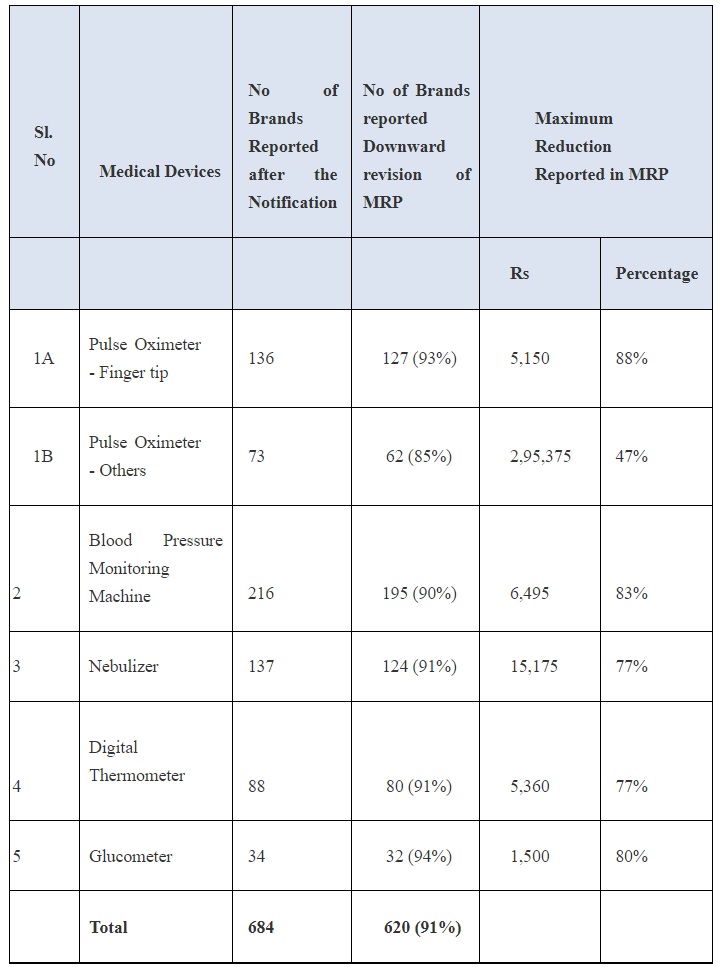
The downward revision of MRP has been reported by imported and domestic brands across all the categories. The highest reduction in prices for Pulse Oximeters, Blood Pressure Monitoring Machine and Nebulizer has been reported by importers.
The revised MRP effective from 20th July 2021 on all the brands and specifications has been shared with the State Drug Controllers for strict monitoring and enforcement. The relevant instructions are available on NPPA’s website (www.nppa.gov.in). In order to monitor availability, the manufacturers / importers of these medical devices have been directed to submit quarterly stock details.
This significant move has received support from Industry Associations like FICCI, AdvaMed, and AMCHAM.
Dr Rajesh Sagar, Professor, Department of Psychiatry, All India Institute of Medical Sciences (AIIMS) New Delhi and Member, Central Mental Health Authority explains the impact of the pandemic on the mental health of children and how it can be addressed.
How has the pandemic affected children’s mental health?
Children are delicate—physically as well as psychologically. Any form of stress, worry, trauma can affect them deeply and lead to long-lasting repercussions. The pandemic has altered their normal activities—their schools are shut; the education has shifted to online and their interaction with peers is restricted and limited. Besides, there are some who have lost one or both parents or relatives or caregivers.
All these factors can affect the mental wellbeing of children, depriving them of the emotionally fulfilling environment, important for their normal growth and development.
What is the biggest challenge you face while dealing with distressed children?
Unlike adults, children react differently in stressful situations. Some children become clingy, some are withdrawn, some become aggressive, some depressed. So, it is difficult to understand the mental state of children. What we know is the fact that the surrounding environment affects the emotion or moods of children. At times, children internalise a situation. Panic, illness, or death of near and dear ones can affect them adversely and at times, they may not be able to express their fears, anxiety, or worries.
So, it is important for adults to keep a watch on the behaviour of children. During the current crisis, it is also important that adults encourage children to communicate their views, and perspectives on various issues related to them. For children to be able to express themselves clearly, they must be provided with an enabling environment. If they are unable to talk, they can be encouraged to express themselves through drawing, paintings, and other mediums. The impact of the pandemic on children cannot be addressed with direct questions; caregivers need to be gentle while communicating with children as they may be unaware of what is happening to them internally. So, it is important to encourage usage of creative ways in understanding them but communicate directly when discussing difficult topics, like infection, death, and so on.
The first five-six years of a child’s life are said to be the foundational years when a child requires various stimuli for normal growth and development. How is pandemic affecting younger children and how do you think the effect can be minimised?
The first five years, indeed, are very crucial in a child’s life and we need to provide the child multi-modal stimulus. Lack of a positive environment, lack of stimulation, or social interactions can affect them adversely. Though we cannot put children at risk of catching the infection, we need to build a fun-filled, environment where children can be engaged in various activities. Even online education should focus on activity-based learning. I strongly feel that we need to devise methods that are enjoyable and safe as well so that we can minimise the impact of the pandemic on children.
Older children too are facing uncertainty on the academic front. What will be your advice for them?
It is normal for them to feel uncertain. The pandemic has disrupted their education and career plans. Here the role of the parents, caregivers, or teacher becomes very crucial. They need to guide the children that there is not much we can do about the situation, and they are not in it alone, rather there are many other children across the globe who are facing a similar dilemma. It is also important for the parents to accept the reality and pass it on to the children while supporting them throughout the process. The education boards are being flexible in taking exams and so, I think, we will reach a point when this virus will not impact their education and career choice so adversely.
The pandemic has put a special focus on parenting. How would you counsel parents?
With the fine line between the workspace and personal space blurring, many parents are finding it difficult to deal with the added responsibility of looking after the academic needs of their children. Children of every age group have different needs—they need, time, attention, engagement, resources, and a happy environment. A stressful environment at home can be a trigger for a mental health condition, but a safe environment can protect them from existing mental health concerns.
For parents to be able to engage children, they need to be in a positive frame of mind themselves. Parents need to find ways to calm themselves. They need to streamline their daily activities so that they can take out time for children.
Those who are unable to cope with the stress should seek support from family, friends, or professionals.
Government of India, under NHM, provides for technical and financial support to the States/UTs for improving their health care systems in rural and remote areas.
Total of 5 lakh Ayushman Bharat- Health & Wellness Centers (HWCs) are being set up especially in villages and remote areas by upgrading Sub-Centers (SCs) & Primary Health Centers (PHCs) for delivering comprehensive primary health care, closer to the homes of the people.
Accordingly, 77,284 HWCs have become functional with this support. The basic facility available through HWCs are at Annexure-I.
Government of India through the Emergency Response and Health System Preparedness package (ECRP) has extended support to the states/UTs for managing the current and future imminent wave of COVID-19.
In addition to the above, Prime Minister Atmanirbhar Swasth Bharat Yojana (PMASBY) Scheme has been announced in the budget FY 21-22, focusing on developing capacities of health systems and institutions across the continuum of care at all levels viz. primary, secondary and tertiary and on preparing for future pandemics/disasters. Details of PMASBY are at Annexure-IV
Health Wellness Centres
HWCs are providing a package of following 12 services to make basic health facilities equitable, accessible, affordable to under-served people especially in rural and remote areas:
Care in Pregnancy and Child Birth.
Neonatal and Infant health care services.
Childhood and Adolescent health care services.
Family planning, contraceptive services and other reproductive health care services Management of communicable diseases: National Health programmes
General out-patient care for acute simple illnesses and minor ailments
Screening, prevention, control and management of non-communicable diseases and chronic communicable diseases like tuberculosis and leprosy Basic oral health care
Screening and basic management of mental Health ailments
Care for common ophthalmic and ENT problem
Elderly and palliative health care services
Emergency medical services including burns and trauma.
In addition to the above there are a range of wellness activities which include the following:
Regular Yoga sessions / Wellness sessions.
Through Annual Health Calendar, 39 Health days have been identified to conduct health promotion activities.
Ayushman Bharat -Health and Wellness Ambassador Initiative has been launched wherein two teachers in every school will be Ambassadors to foster growth, development and educational achievement of school going children by promoting their health and wellbeing. This is joint initiative of MoHFW and MHRD under comprehensive School Health Program (SHP).
Eat-Right toolkit and Food Safety kit (Magic Box) have been developed in collaboration with FSSAI, under the initiative ‘SahiBhojanBehtarJeevan’ (सहीभोजनबेहतरजीवन) Eat Right India’
India COVID-19 Emergency Response & Health System Preparedness Package (ECRP-I)
Health Infrastructure for Covid-19 Treatment
ECRP-I for Rs. 15,000 Crore (USD 2 billion) has been released to all states/UTs in April 2021 to prevent, detect and respond to the threat posed by COVID-19. Under the package, so far, a total of Rs.13719.22 Cr of committed expenditure has been reported by the implementation agencies. Rs.8147.29 Cr has been released to the States/UTs to prevent, detect, and respond to the threat posed by COVID-19.
To equip existing health facilities and to set up additional facilities resources are being made available. Dedicated hospitals have been set up for meeting the COVID-19 health emergency.
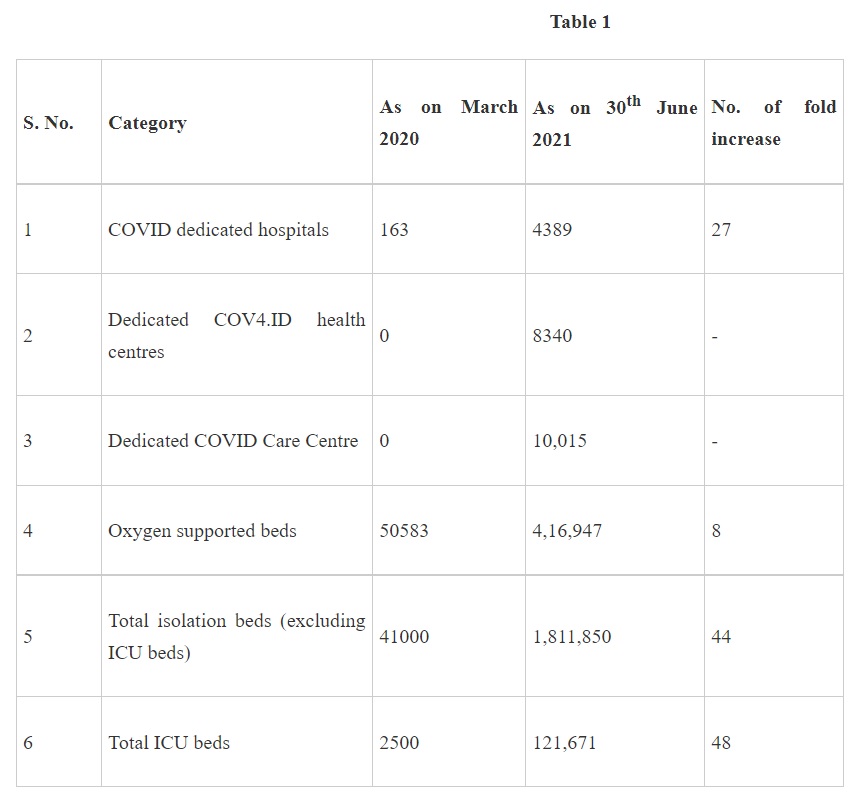
India COVID-19 Emergency Response & Health System Preparedness Package (ECRP-II)
ECPP- II for Rs. 23,123 Crore has been approved by Cabinet on 8th July 2021 and the amount is being released to the states, with an aim to strengthening district and sub district capacity for an effective and rapid response to the pandemic.
Support is available for States/UTs to:
Under India Covid-19 Emergency Response and Health Systems Preparedness Package - Phase-II”(ECRP-Phase-II) during 2021-22, approved by the Cabinet on 8.07.2021, an amount of Rs.23,123 crores, is earmarked for implementing the scheme in 9 months from 1st July, 2021 to 31st March, 2022. The Scheme is aimed to prevent, detect and strengthen national health systems, respond to the continuing threat posed by COVID-19 in India. The scheme is a Centrally Sponsored Scheme (CSS) with some Central Sector (CS) components.
Create Paediatric units in all districts (42 or 32 bedded units including Oxygen Supported beds and ICU beds)and also, to establish Paediatric Centre of Excellence (Paediatric CoE) in each State/UT, (either in Medical Colleges, State Govt. Hospitals or Central Hospitals such as AIIMS, INIs, etc) for providing Tele-ICU services, mentoring and technical hand-holding to the District Paediatric units
Establishing 6 bedded units at Sub Health Centres and Primary Health Centres and 20 bedded units at Community Health Centres for meeting the requirement beds inperi-urban and tribal areas.
Besides, the support is provided to provision of required drugs and diagnostics for COVID management, including maintaining a buffer stock for essential medicines required for effective COVID-19 management. Further, support is extended to establish Field Hospitals (100 bedded or 50 bedded units) wherever required.
Augment ICU beds in public healthcare system out of which 20% will be Pediatric ICU beds.
Provide care closer to the community due to the ingress of COVID-19 in rural, peri-urban and tribal areas, by creating pre-fabricated structures for adding additional beds at the existing CHCs, PHCs and SHCs (6-20 bedded units) and support would also be provided to establish bigger field hospitals (50-100 bedded units) depending on the needs at tier-II or Tier-III cities and district HQs.
Install Liquid Medical Oxygen Storage Tanks with Medical Gas Pipeline System (MGPS), with an aim to support at least one such unit per district.
Augment the existing fleet of ambulances especially ALS ambulances to ensure at least one ALS ambulance is available in each block.
Engage Final year MBBS students, Interns, Post Graduate Residents and final year BSc, & GNM nursing students for effective COVID management.
As “Test, Isolate and Treat” and following COVID Appropriate Behaviour at all the times, is the national strategy for effective COVID-19, support will be available to the States to maintain at least 21.5 lakhs tests per day.
Flexible support to the Districts for meeting the requirement of essential medicines for COVID-19 management, including creation of buffer stock.
Guidance Note on “India Covid-19 Emergency Response and Health Systems Preparedness Package - Phase-II” (ECRP-Phase-II) has been shared with the States/UTs on 14th July 2021, requesting the States to send the proposals for appraisal and approval.
15% of amount of Central Share of CSS components of ECRP-II (Rs.1,827.8 Cr) has been released to 36 States/UTs on 22nd July 2021, as an advance to enable the States/UTs to ensure implementation of critical activities.
Prime Minister AtmanirbharSwasth Bharat Yojana (PMASBY)
Prime Minister AtmanirbharSwasth Bharat Yojana (PMASBY) Scheme has an outlay of about Rs. 64,180 Cr over six years (to be implemented till 2025-26) Under PMASBY efforts to enhance public health capacities are being undertaken like the following:
A paradigm shift in provision of Urban Primary Health Care services with establishment of 11,024 new urban Health and Wellness Centers across the country with a focus on slum and slum like areas
Infrastructure support for 17,788 AB- Health and Wellness Centres in rural areas in seven High Focus States and three NE States.
Setting up of 3,382 Block Public Health Units (BPHUs) in 11 High Focus States/UTs to strengthen Public Health functions such as surveillance, epidemiological investigations along with enhanced capacities for clinical diagnostic services and
Establishment / Strengthening of Integrated District Public Health Labs (IPHLs) in all 730 districts.
Establishment of 50/100 bedded Critical Care Hospital Blocks in 602 Districts and 150 bedded Critical Care Hospital Blocks in 12 AIIMS and Central Institutions.
Health Emergency Response- Two state-of-the-art Self-contained container based mobile hospitals and 15 Health Emergency Operation Centres (HEOCs) towards strengthening Disaster and Epidemic Preparedness and response
The Cabinet note for this scheme has been circulated and it is awaiting the approval of the Cabinet.
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Lok Sabha here today.
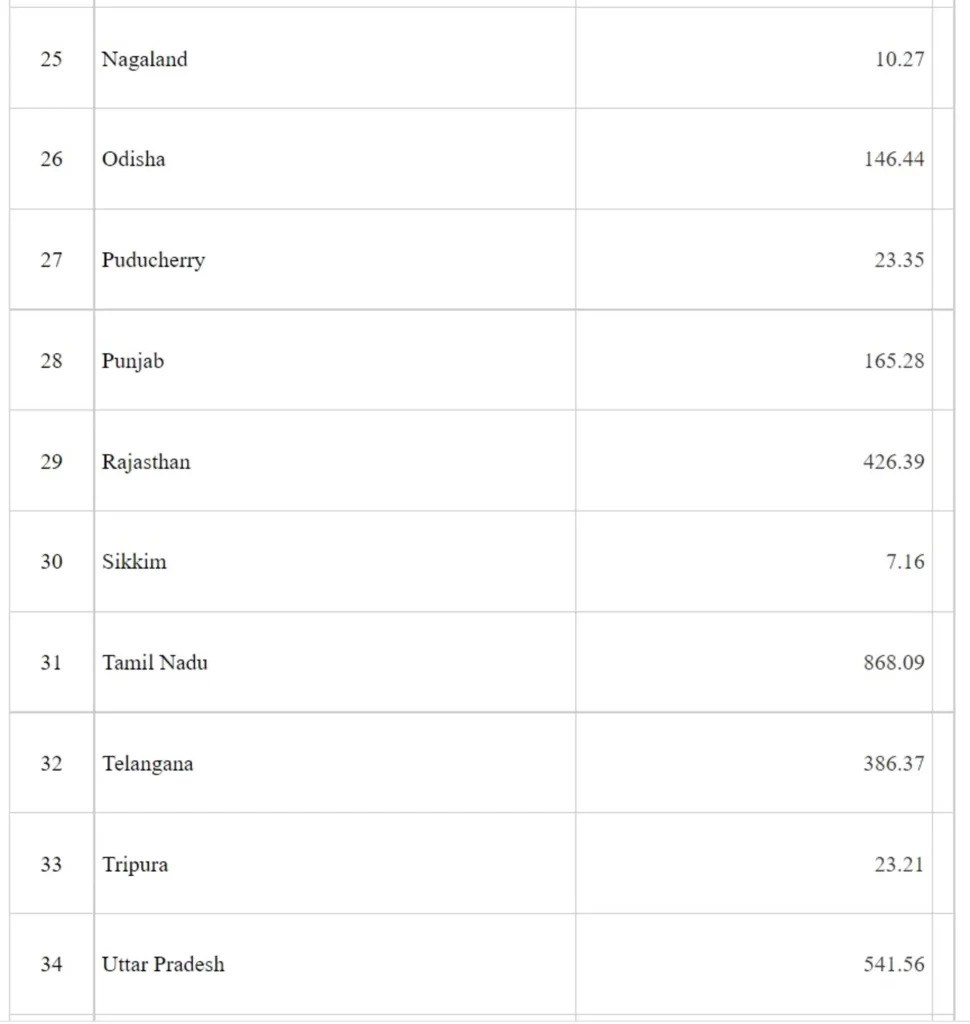
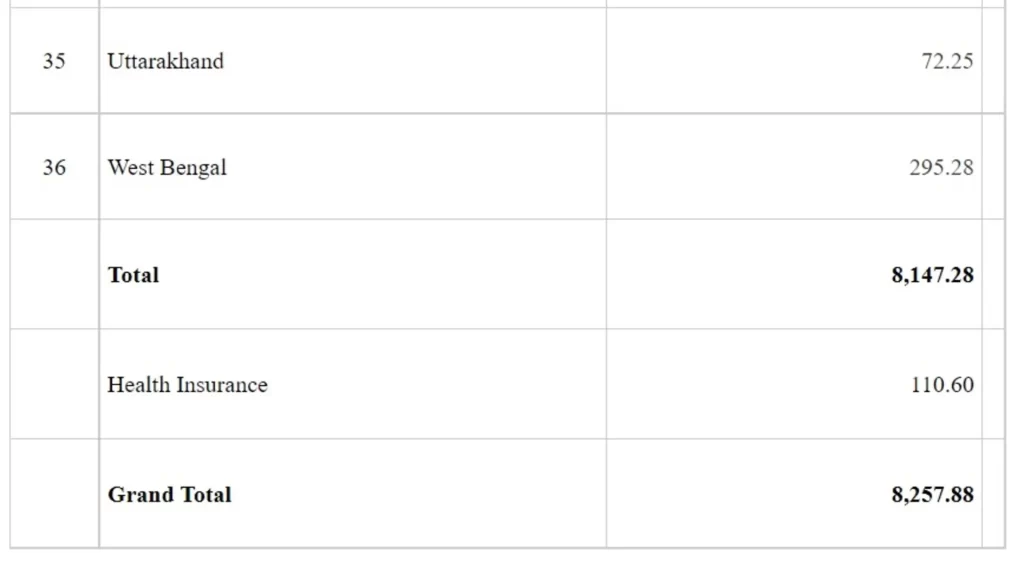
All the States/UTs are provided with necessary financial support to check the COVID-19 Pandemic.Under India COVID-19 Emergency Response and Health System Preparedness Package, an amount of Rs 15,000 Cr has been approved by Cabinet on 22nd April 2020.
Under the Package, during the FY 2020-21, funds to the tune of Rs 8257.88 Cr have been released to the State/UTs through National Health Mission (NHM) framework. Rs 8257.88 Cr includes Rs 110.60 Cr towards payment of insurance of health workers. State-wise details are given at Annexure -I.
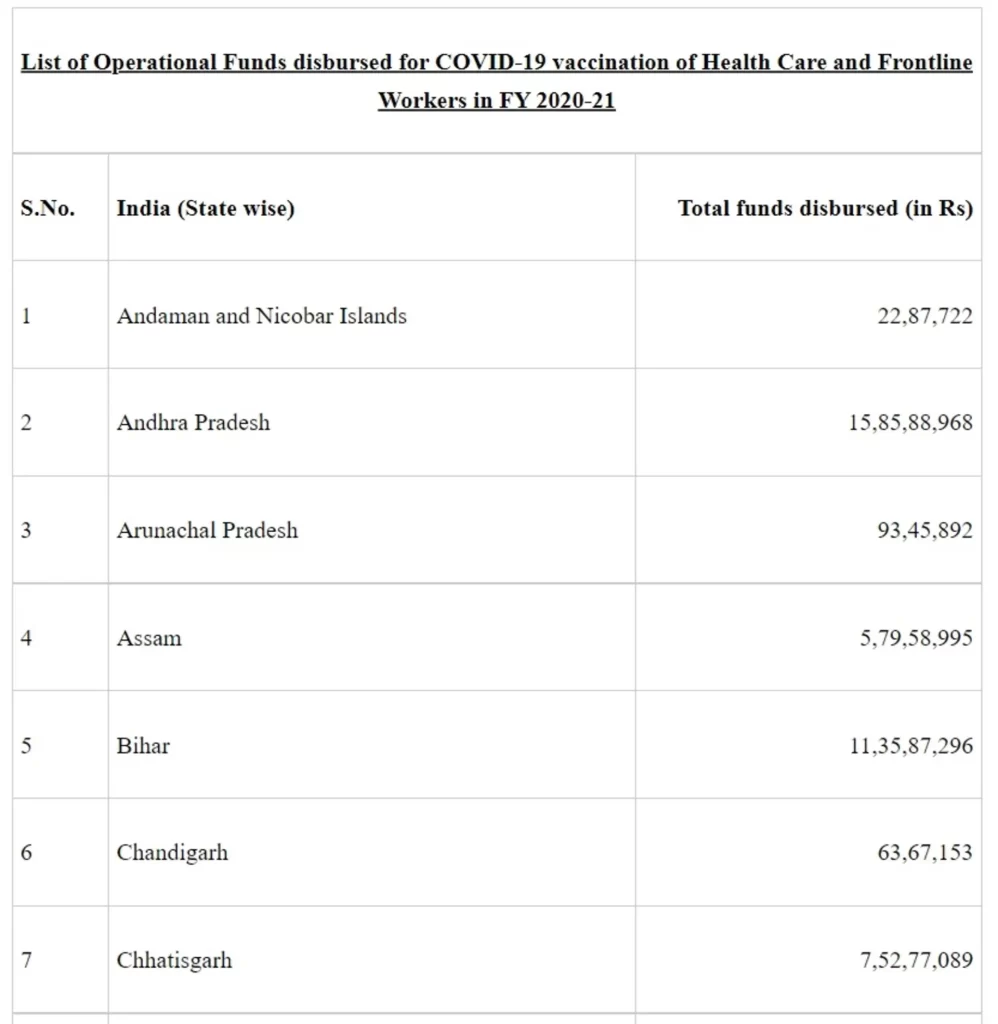
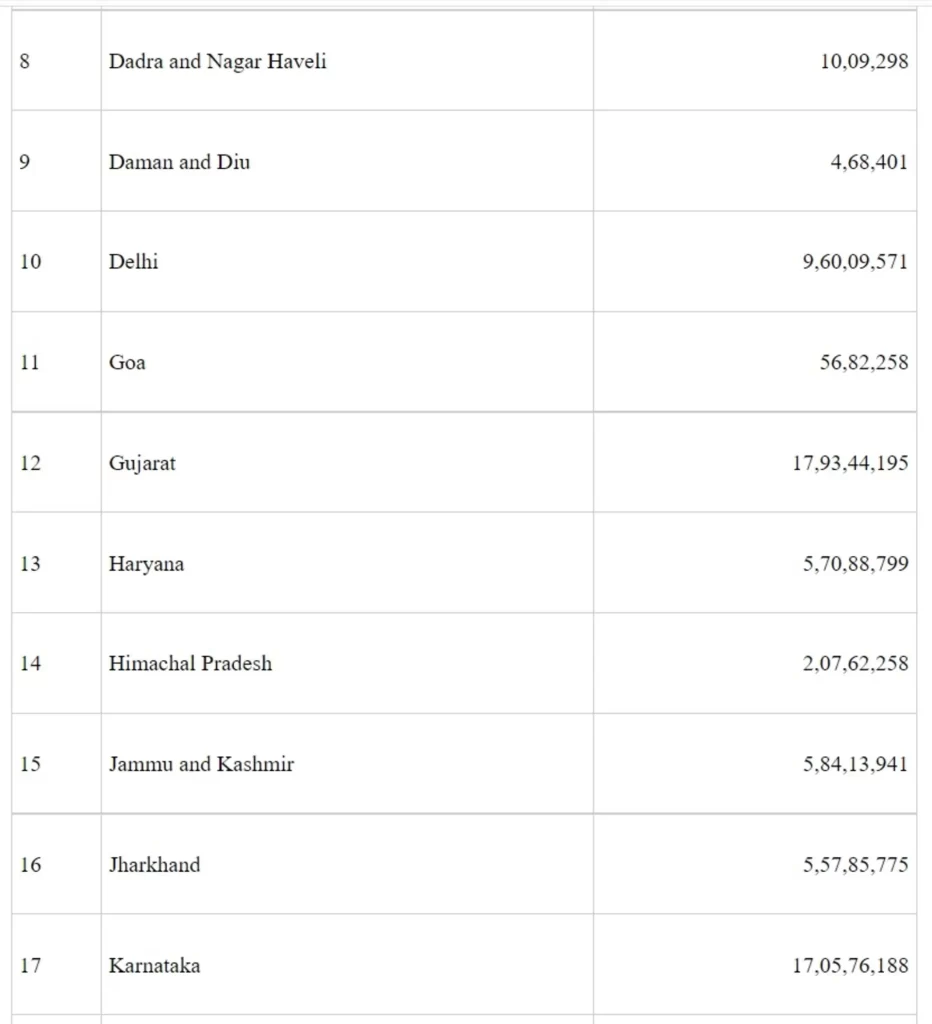
Further, Operational cost was provided to States/UTs for vaccination of Health Care Workers and Front-Line Workers under COVID-19 Vaccination Drive in the financial year 2020-21. State-wise details are given at Annexure -II.
A database of relief material donated by different countries for COVID19 management during the second wave has been maintained. The item- and country-wise details can be accessed atMoHFW website (link: https://main.mohfw.gov.in/node/5551). The same have been distributed to all States/UTs of the country.
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Lok Sabha here today.
Annexure-I
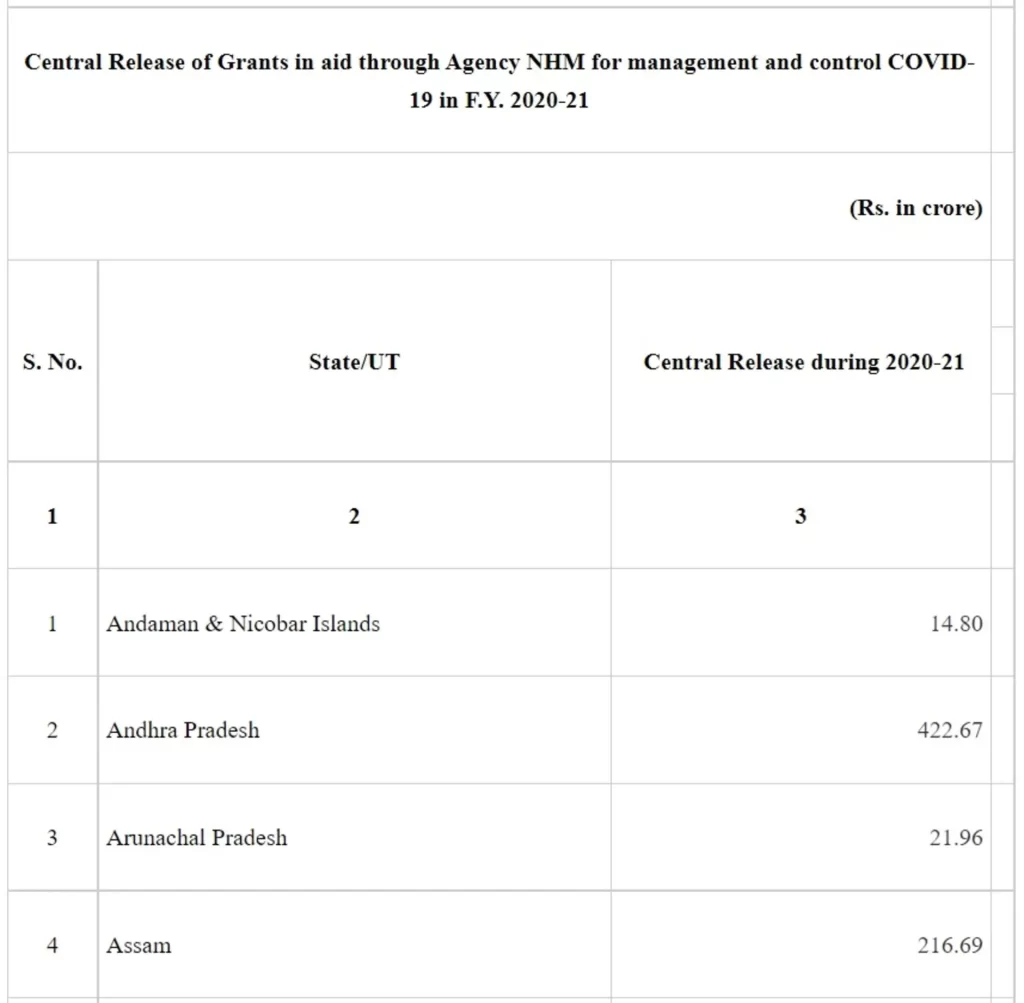

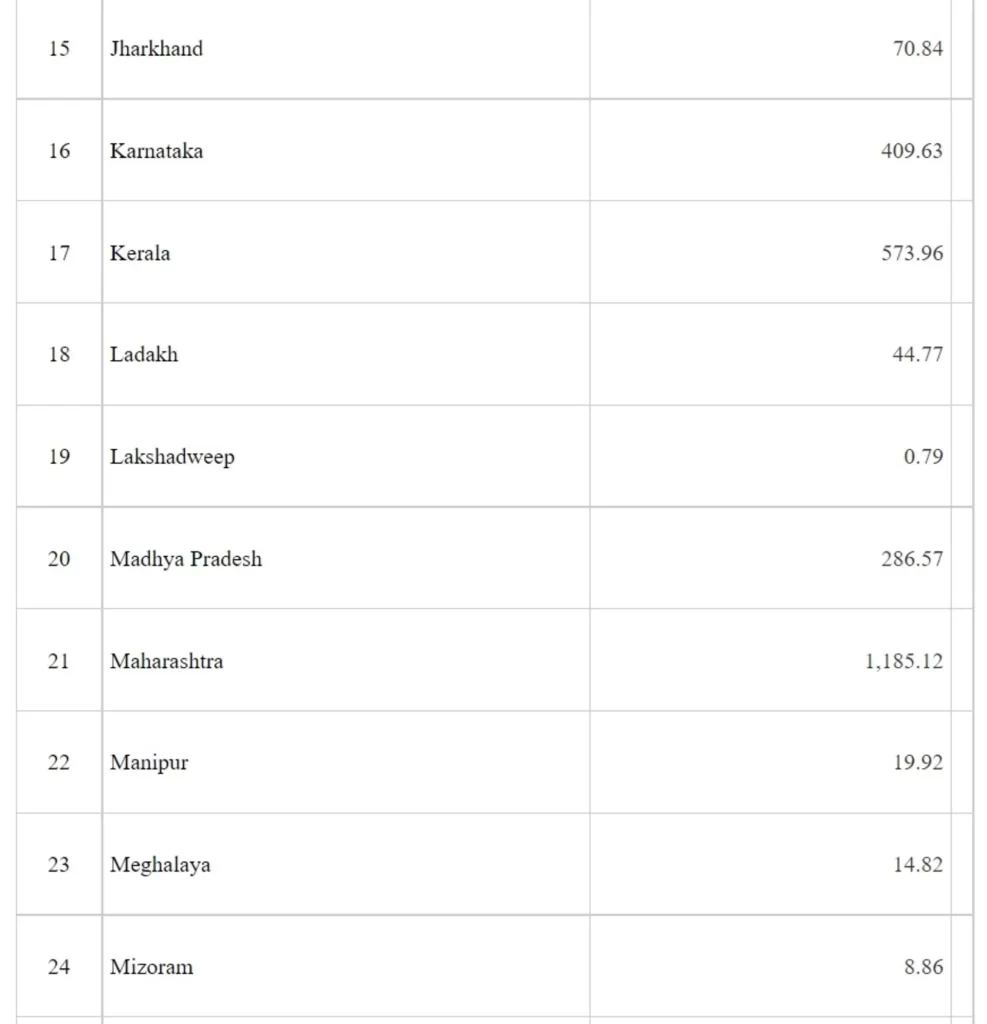
Annexure II
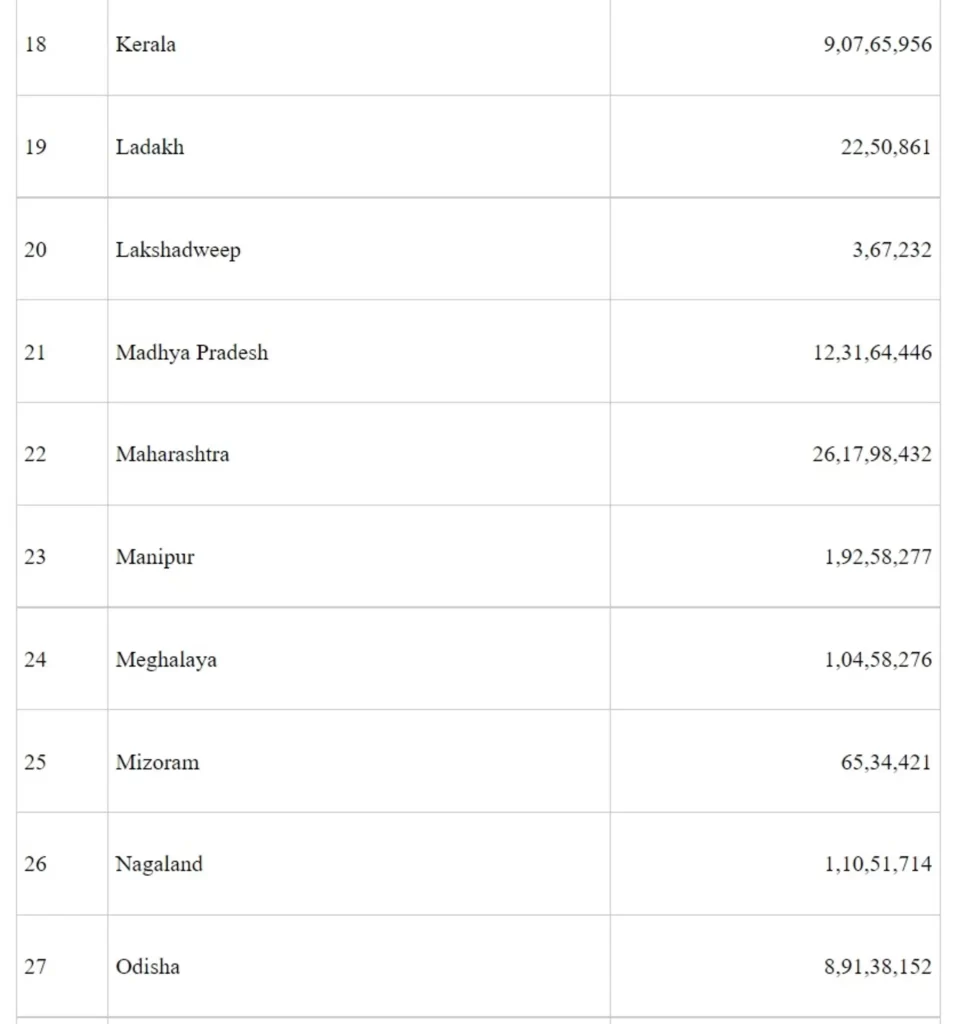
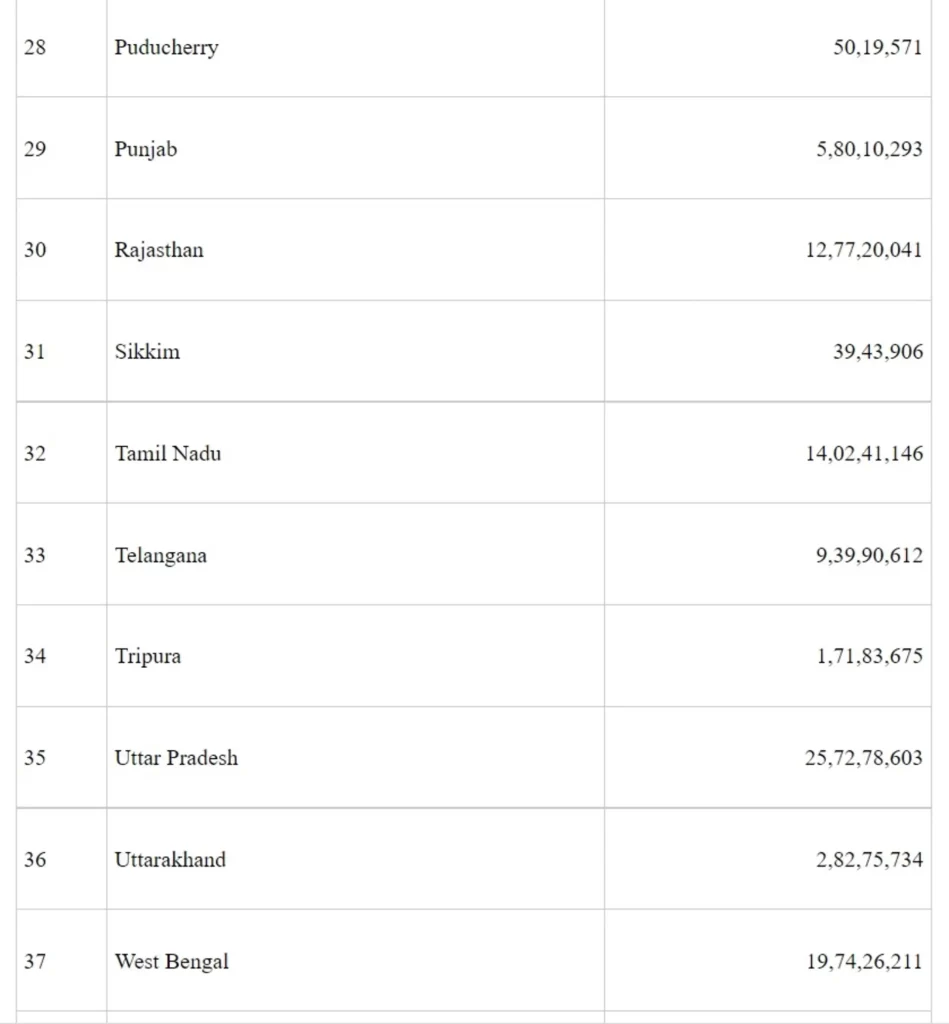
National Policy for Rare Diseases, 2021 (the Policy) has been finalized and put in public domain.
The Policy can be accessed at website- https://main.mohfw.gov.in/documents/policy.
The Policy aims at lowering the incidence and prevalence of rare diseases based on an integrated and comprehensive preventive strategy encompassing awareness generation, premarital, post-marital, pre-conception and post-conception screening and counselling programmes to prevent births of children with rare diseases, and within the constraints on resources and competing health care priorities, enable access to affordable health care to patients of rare diseases.
Initiatives for treatment support for patients of rare diseases under the Policy are as follows: -
i. Financial support up to Rs. 20 lakhs under the Umbrella Scheme of Rashtriya Arogaya Nidhi shall be provided by the Central Government for treatment, of those rare diseases that require a one-time treatment (diseases listed under Group 1). Beneficiaries for such financial assistance would not be limited to BPL families, but extended to about 40% of the population, who are eligible as per norms of Pradhan Mantri Jan Arogya Yojana, for their treatment in Government tertiary hospitals only.
ii. State Governments can consider supporting patients of such rare diseases that can be managed with special diets or hormonal supplements or other relatively low-cost interventions (Diseases listed under Group 2).
iii. Keeping in view the resource constraints, and a compelling need to prioritize the available resources to get maximum health gains for the community/population, the Government will endeavour to create alternate funding mechanism through setting up a digital platform for voluntary individual and corporate donors to contribute to the treatment cost of patients of rare diseases.
iv. Voluntary crowd-funding for treatment: Keeping in view the resource constraint and competing health priorities, it will be difficult for the Government to fully finance treatment of high-cost rare diseases. The gap can however be filled by creating a digital platform for bringing together notified hospitals where such patients are receiving treatment or come for treatment, on the one hand, and prospective individual or corporate donors willing to support treatment of such patients. The notified hospitals will share information relating to the patients, diseases from which they are suffering, estimated cost of treatment and details of bank accounts for donation/ contribution through online system. Donors will be able to view the details of patients and donate funds to a particular hospital. This will enable donors from various sections of the society to donate funds, which will be utilized for treatment of patients suffering from rare diseases, especially those under Group 3. Conferences will be organized with corporate sector companies to motivate them to donate generously through digital platform. Ministry of Corporate Affairs will be requested to encourage PSUs and corporate houses to contribute as per the Companies Act as well as the provisions of the Companies (Corporate Social Responsibility Policy) Rules, 2014 (CSR Rules). Promoting health care including preventive health care is included in the list in the Schedule for CSR activities.
Treatment cost of the patient will be first charge on this fund. Any leftover fund after meeting treatment cost can be utilized for research purpose also.
At present financial assistance to poor patients, living below threshold poverty line and also to the population, who are eligible as per norms of Pradhan Mantri Jan Arogya Yojana under Ayushman Bharat, suffering from specified rare diseases for their treatment at Government Hospitals or Institutes having super specialty facilities / Government tertiary hospitals is being provided under the Umbrella Scheme of Rashtriya Arogya Nidhi (RAN). The budget allocation for the current financial year 2021-2022 for rare diseases is Rupees 25 Crore.
National Policy for Rare Diseases, 2021 provides for National Consortium for Research and Development on therapeutics for Rare Diseases with an expanded mandate to include research & development, technology transfer and indigenization of therapeutics for rare diseases. It will be convened by Department of Health Research (DHR) with ICMR as a member.
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Lok Sabha here today.
Dr Rajesh Sagar, Professor, Department of Psychiatry, All India Institute of Medical Sciences (AIIMS) New Delhi and Member, Central Mental Health Authority explains the impact of the pandemic on the mental health of children and how it can be addressed.
How has the pandemic affected children’s mental health?
Children are delicate—physically as well as psychologically. Any form of stress, worry, trauma can affect them deeply and lead to long-lasting repercussions. The pandemic has altered their normal activities—their schools are shut; the education has shifted to online and their interaction with peers is restricted and limited. Besides, there are some who have lost one or both parents or relatives or caregivers.
All these factors can affect the mental wellbeing of children, depriving them of the emotionally fulfilling environment, important for their normal growth and development.
What is the biggest challenge you face while dealing with distressed children?
Unlike adults, children react differently in stressful situations. Some children become clingy, some are withdrawn, some become aggressive, some depressed. So, it is difficult to understand the mental state of children. What we know is the fact that the surrounding environment affects the emotion or moods of children. At times, children internalise a situation. Panic, illness, or death of near and dear ones can affect them adversely and at times, they may not be able to express their fears, anxiety, or worries.
So, it is important for adults to keep a watch on the behaviour of children. During the current crisis, it is also important that adults encourage children to communicate their views, and perspectives on various issues related to them. For children to be able to express themselves clearly, they must be provided with an enabling environment. If they are unable to talk, they can be encouraged to express themselves through drawing, paintings, and other mediums. The impact of the pandemic on children cannot be addressed with direct questions; caregivers need to be gentle while communicating with children as they may be unaware of what is happening to them internally. So, it is important to encourage usage of creative ways in understanding them but communicate directly when discussing difficult topics, like infection, death, and so on.
The first five-six years of a child’s life are said to be the foundational years when a child requires various stimuli for normal growth and development. How is pandemic affecting younger children and how do you think the effect can be minimised?
The first five years, indeed, are very crucial in a child’s life and we need to provide the child multi-modal stimulus. Lack of a positive environment, lack of stimulation, or social interactions can affect them adversely. Though we cannot put children at risk of catching the infection, we need to build a fun-filled, environment where children can be engaged in various activities. Even online education should focus on activity-based learning. I strongly feel that we need to devise methods that are enjoyable and safe as well so that we can minimise the impact of the pandemic on children.
Older children too are facing uncertainty on the academic front. What will be your advice for them?
It is normal for them to feel uncertain. The pandemic has disrupted their education and career plans. Here the role of the parents, caregivers, or teacher becomes very crucial. They need to guide the children that there is not much we can do about the situation, and they are not in it alone, rather there are many other children across the globe who are facing a similar dilemma. It is also important for the parents to accept the reality and pass it on to the children while supporting them throughout the process. The education boards are being flexible in taking exams and so, I think, we will reach a point when this virus will not impact their education and career choice so adversely.
The pandemic has put a special focus on parenting. How would you counsel parents?
With the fine line between the workspace and personal space blurring, many parents are finding it difficult to deal with the added responsibility of looking after the academic needs of their children. Children of every age group have different needs—they need, time, attention, engagement, resources, and a happy environment. A stressful environment at home can be a trigger for a mental health condition, but a safe environment can protect them from existing mental health concerns.
For parents to be able to engage children, they need to be in a positive frame of mind themselves. Parents need to find ways to calm themselves. They need to streamline their daily activities so that they can take out time for children.
Those who are unable to cope with the stress should seek support from family, friends, or professionals.
“Public Health and Hospitals” being a State subject, the primary responsibility of strengthening public healthcare system, including for provision of quality healthcare and advanced treatment and diagnostic facilities, lies with the respective State Governments. However, under National Health Mission (NHM), technical and financial support is provided to the States/UTs to strengthen the public healthcare delivery at public healthcare facilities.
To address the healthcare challenges, particularly in rural areas, the National Rural Health Mission (NRHM) was launched in 2005 to supplement the efforts of the State/UT governments to provide accessible, affordable and quality healthcare to all those who access public health facilities. Currently, NRHM is a sub-mission of National Health Mission (NHM). NUHM was also launched in 2013 as a sub-mission of NHM.
NHM support is provided to States/ UTs for setting up of new facilities as per norms and upgradation of existing facilities for bridging the infrastructure gaps based on the requirement posed by them.
NHM support is also provided for provision of a range of free services related to maternal health, child health, adolescent health, family planning, universal immunisation programme, and for major diseases such as Tuberculosis, vector borne diseases like Malaria, Dengue and Kala Azar, Leprosy etc.
Other major initiatives supported under NHM include Janani Shishu Suraksha Karyakram (JSSK) (under which free drugs, free diagnostics, free blood and diet, free transport from home to institution, between facilities in case of a referral and drop back home is provided), Rashtriya Bal Swasthya Karyakram (RBSK) (which provides newborn and child health screening and early interventions services free of cost for birth defects, diseases, deficiencies and developmental delays to improve the quality of survival), implementation of Free Drugs and Free Diagnostics Service Initiatives, PM National Dialysis Programme and implementation of National Quality Assurance Framework in all public health facilities including in rural areas.
Mobile Medical Units (MMUs) & Tele-consultation services are also being implemented to improve access to healthcare particularly in rural areas.
As part of Ayushman Bharat, the States are supported for establishment of 1.5 lakh Health and Wellness Centres across the country by December, 2022 for provision of comprehensive primary care that includes preventive healthcare and health promotion at the community level with continuum of care approach. Further Ayushman Bharat, Pradhan Mantri Jan Arogya Yojana (AB-PMJAY) provides health coverage up to Rs 5 Lakh per family per year to around 1074 crore poor and vulnerable families as per Socio Economic Caste Census (SECC).
In the 15 years of implementation, the NHM has enabled achievement of the Millennium Development Goals (MDGs) for health. It has also led to significant improvements in maternal, new-born, and child health indicators, particularly for maternal mortality ratio, infant and under five mortality rates, wherein the rates of decline in India are much higher than the global averages and these declines have accelerated during the period of implementation of NHM. The major achievements under NHM are given at Annexure.
Improvements in Core Health Outcomes:
Reduction in OOPE: The average medical expenditure per hospitalization and childbirth also declined in this period, from Rs. 5636 to Rs. 4290 in rural areas, and Rs. 7670 to Rs. 4837 in urban areas for hospitalization and from Rs. 1587 to Rs. 1324 in rural areas and Rs. 2117 to Rs. 1919 in urban areas for institutional delivery, indicating the impact of NHM in reduction of Out of Pocket Expenditures for health care.
Maternal Mortality Rate (MMR) has declined from 556/lakh live births in 1990 to 113/lakh live births in 2016-2017. Rate of decline of MMR in India at 77% is much higher than global average decline of 44% over the same period.
Infant Mortality Rate (IMR), declined from 80 in 1990 to 32 in the year 20181.
Under 5 Mortality Rate (U5MR), declined from 52 in 2012 to 36 in 2018,
Total Fertility Rate (TFR) declined from 2.3 in 2013 to 2.2 in the year 20181.
The incidence of Tuberculosis per 1,00,000 population reduced from 234 in 2012 to 193 in 2019. The mortality due to TB per 1,00,000 population also reduced from 42 in 2012 to 33 in 2019.
The number of districts that achieved the target of leprosy elimination increased from 543 districts in 2011-2012 to 554 by March 2017 and to 571 districts by March 2018. The prevalence rate of Leprosy reduced to less than 1/10000 population in 610 Districts in 2020.
For Malaria, Annual Parasitic Index (API) was sustained at levels of less than 1 and declined from 0.89 in 2014 to 0.32 in 2018, and 0.25, in 2019. Malaria cases and deaths declined from 21.27% and 20% respectively in 2019 from 2018.
By the end of December 2019, 94% Kala-azar endemic blocks have achieved the elimination target of <1 KA case per 10,000 population at block level.
The National target for sustaining Dengue related case fatality rate to less than 1% was met. Dengue related case fatality rate in 2014 was 0.3% and reduced to 0.1% in 2019.
The prevalence of blindness (visual acuity <3/60) has reduced to 0.36% in 2019) from 0.68% in 2010.
There is a 17.3% relative reduction in prevalence of tobacco use from 34.6% to 28.6% from 2009-10 to 2016-17.
Increased Access to Health Services:
As a result of the health systems strengthening efforts of NHM, the proportion of those seeking care from public health facilities, increased from 28.3% to 32.5% in rural areas and 21.2% to 26.2% in urban areas between 2014 to 2017.; and utilization of public health facilities for institutional deliveries increased from 56% to 69.2% in rural areas and from 42% to 48.3% in urban areas.
Growth in Public Health Facilities:
NHM adopts a health system approach and targets to build a network for public health facilities with Health & Wellness Centres at the grassroot level and District Hospitals, with robust referral linkage, to offer Comprehensive primary and secondary care services to citizens. The growth in the number of facilities at various levels since 2025 is given in Table 1 -
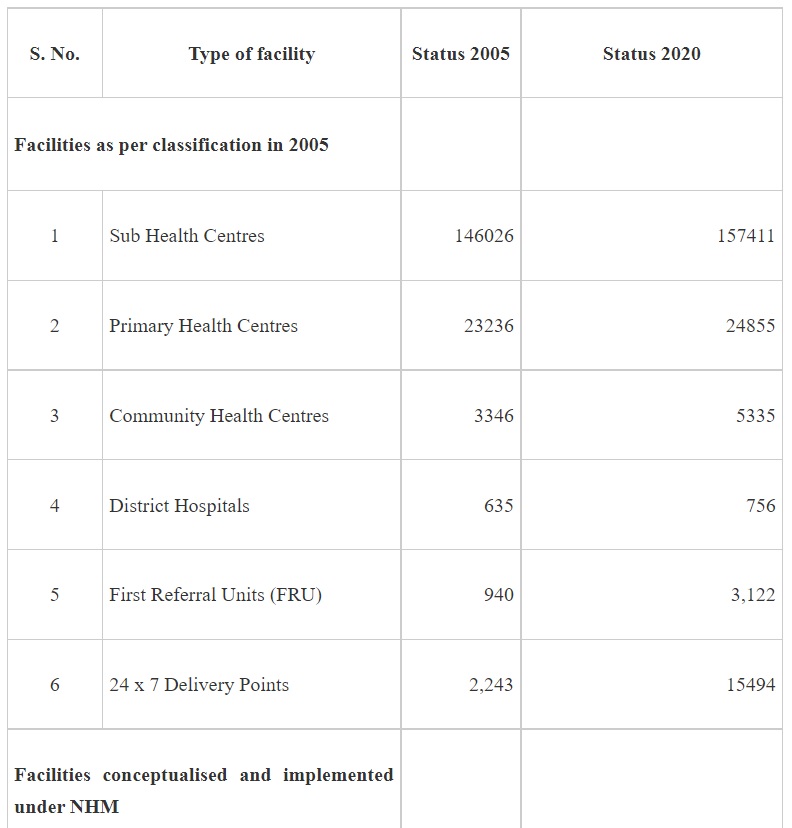
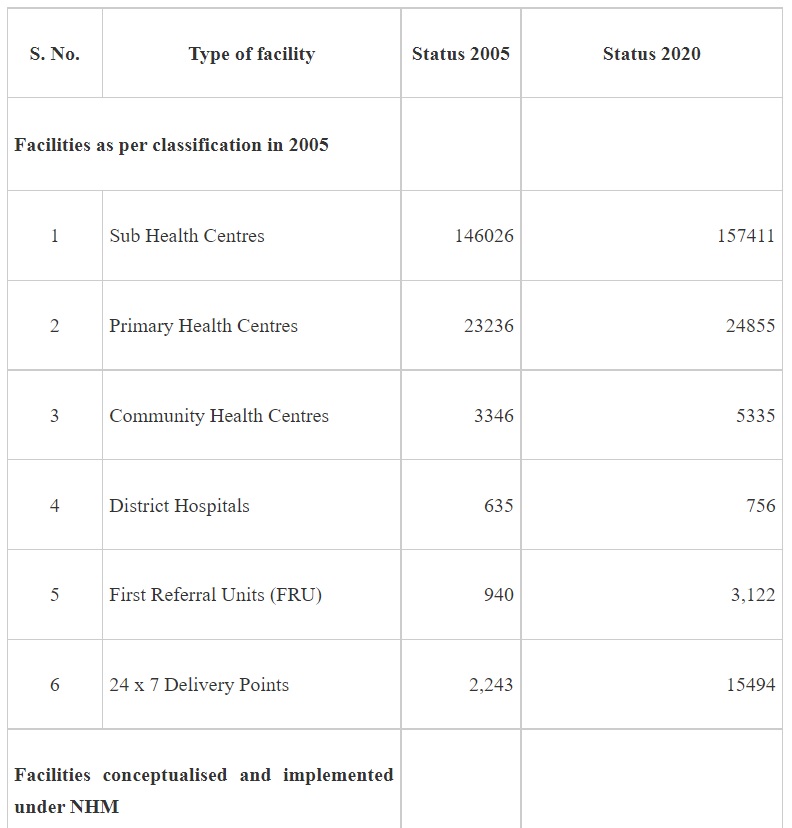
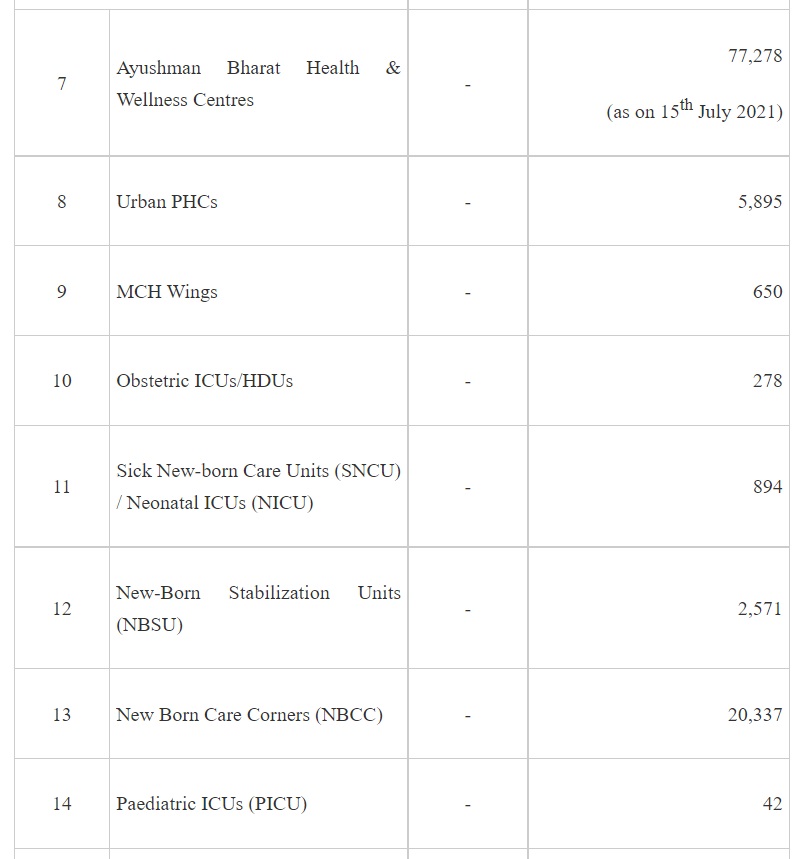

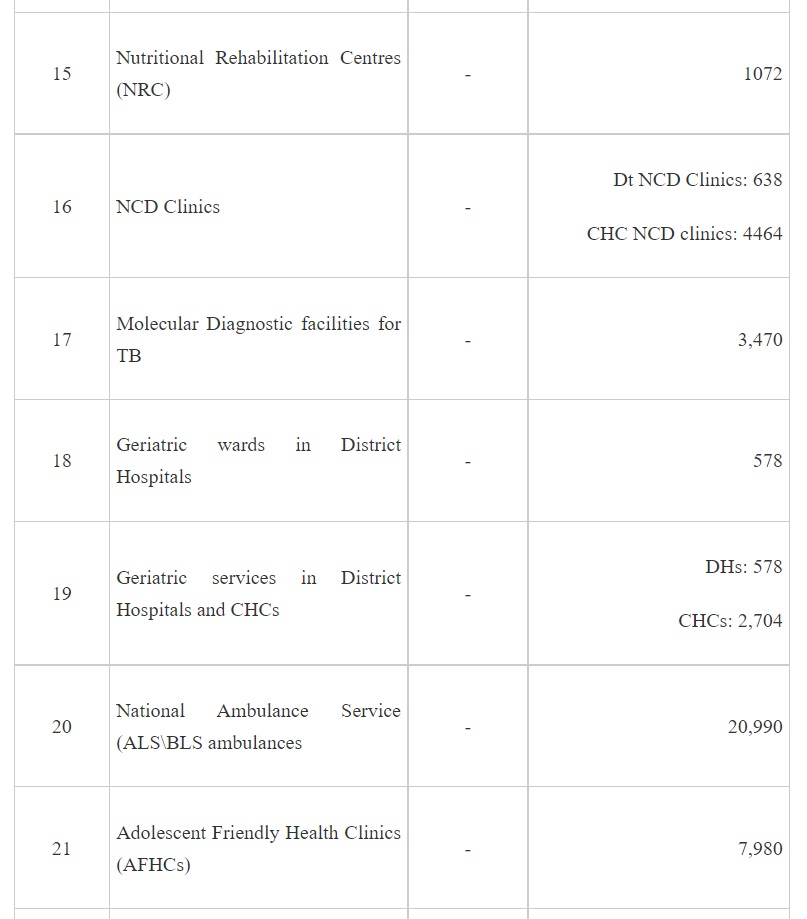
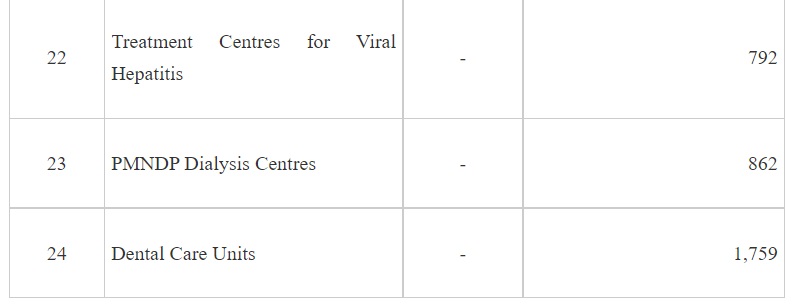
It may be seen from the above that implementation of NHM has not only contributed to increase in the institutional capacities for service delivery but also has led to development of capacities for targeted interventions of the various National Programmes under the NHM.
3. Equitable development: There was also a sustained focus on the health of tribal populations, those in Left Wing Extremism areas, and the urban poor. A more recent effort at ensuring equity in access and use, is the Aspirational district initiative, in which 115 districts across 28 states, with weak social and human development indicators have been identified for allocation of additional resources and capacity enhancement to catch up with more progressive districts.
4. National Ambulance Services: At the time of launch of NRHM (2005), ambulance networks were non-existent. So far, 20,990 Emergency Response Service Vehicles are operational under NRHM. Besides 5,499 patient transport vehicles are also deployed, particularly for providing “free pickup and drop back” facilities to pregnant women and sick infants.
5. Human Resource Augmentation: NHM supports states for engaging of service delivery HR such as doctors, nurses and health workers and also implements the world’s largest community health volunteer programme through the ASHAs. More than 10 lakhs ASHAs and ASHA facilitators are engaged under NHM. NHM has also supported states to acquire staff with skills in public health, finance, planning, management and M&E to plan and implement interventions, freeing up clinical staff to deliver health services. Differential remuneration and incentives linked to remote/underserved areas of posting, resulted in increased availability and retention of HR in difficult and remote areas. Human Resource Information System (HRIS) is a key administrative HR reform implemented under NHM for regular and contractual staff, providing comprehensive real time information on the HR posted in facilities and in managerial positions, facilitating salary payments and transfer postings. NHM invests in capacity building and mentoring for all cadres of personnel, with a focus on multi-skilling and task sharing to address HR shortages.
6. Health Sector Reforms: The National Health Mission (NHM) enabled the design and implementation of reforms specifically related to Governance (Decentralized Management Units, and creation of flexibility in administrative and fund management decisions, creation of Rogi Kalyan Samitis, establishment of community collectives for accountability, such as the Village Health, Sanitation and Nutrition Committees and Mahila Arogya Samitis), Procurement (creating the institutional mechanisms needed for effective procurement modalities such as the Medical services Corporations in several states, improve supply chain and logistics management, and expand procurement capacity), and Technology (to facilitate reporting, follow up of mothers and children in need of services, IEC and for tracking vaccine use).
7. Addressing high Out-of-Pocket Expenditure (OOPE): Recognising the need for reducing the current high levels OOPE, and that, almost 70% of the OOPE is on account of drugs and diagnostics, the Free Drugs and Free Diagnostics Services Initiatives have been implemented under the NHM. The Essential Drugs Lists (EDL) and the Essential Diagnostics Lists have been notified and are periodically updated to include more essential drugs based on new initiatives undertaken. These interventions coupled with strengthening of health facilities’ capacities to deliver an expanded range of services, closer to communities, teleconsultation services are leading to significant reduction in OOPE.
NHM supported health system reforms have resulted in development of resilient health systems, albeit at different stages of maturity that enable successful scaling up of existing interventions and the addition of newer reforms given the rapid transitions from rural to urban, gradual demographic transition to aging populations, increasing burden of chronic diseases, and the emergence of newer infectious diseases.
Of note is that the NHM reforms were oriented towards addressing inequity, across and within states. A study done in 2020 by the National Institute of Public Finance and Policy (NIPFP) on health spending in states under NHM, suggests that NHM contributed to reduction of inequality in health spending across states and added funds to the lower tiers of the health pyramid.
The Union Minister of State for Health and Family Welfare, Dr. Bharati Pravin Pawar stated this in a written reply in the Rajya Sabha here today.
